In the midst of a raging global pandemic, it is easy to forget that tuberculosis (TB) is the second leading infectious killer after COVID-19 and that ending the TB epidemic by 2030 is among the health targets of the United Nations Sustainable Development Goals (SDGs). In Canada, TB still exists in Indigenous communities, though the rest of the country has been free from it for at least five decades.
In 2018, the federal government committed to eliminating TB from Inuit Nunangat – an area that stretches across the Northwest Territories, Nunavut, northern Quebec and part of Labrador – by 2030. In 2019, the government offered an official apology to the Inuit community for mismanaging the tuberculosis epidemic from the 1940s to the 1960s. To meet the SDG goal and Canada’s commitment to end the TB pandemic by 2030, Canada needs to invest resources to showcase a genuine desire to overcome decades of oppression and failures in the treatment of Indigenous communities.
We learned about the details of the TB pandemic and the associated mistreatment of Indigenous peoples in Canada in the course of our research on colonialism and infectious disease.
This belated discovery of a less-known Indigenous history that is familiar knowledge to Indigenous communities took us back to our childhoods. Despite growing up in different South Asian countries, the two of us, like many people, have been haunted by the 1960 Indian film Meghe Dhaka Tara (The Cloud-Capped Star). The movie forced us to confront the structural conditions of a society that make it impossible for some people to survive TB.
The final moments of this film are impossible to forget. Nita, the main character of Ritwik Ghatak’s movie, is dying of tuberculosis. Her brother is visiting her at the sanatorium when Nita screams her haunting final words: “Dada, ami bachte chai!” or “Brother, I want to live!”
The questions raised by this film have come up for us again here in Canada as our research led us to look at the history of Hamilton, where both of us now live and work, and its connection to the TB pandemic. The Mountain Sanatorium (“the San”), which opened in 1906, was Canada’s fourth sanatorium and by 1932 “one of the largest in the British Empire.”
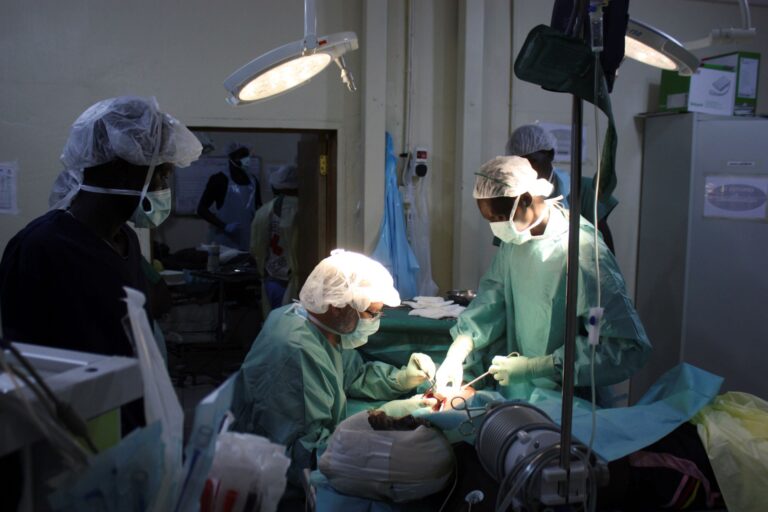
In the 1950s and 1960s, the Canadian government began to send Inuit with TB far from their homes to southern sanatoriums, including in Hamilton, for treatment.
Shawn Selway’s 2016 book Nobody Here Will Harm You, documents the impact on hundreds of Inuit who were uprooted and moved to “the San” between 1950 and 1965. The evacuations split families, and left parents and children wondering about their loved ones. Some of those taken south even died and were buried without their families’ knowledge. Letters home from TB patients in the sanatoriums reveal the miserable living conditions of the Inuit undergoing treatment. Today, that trauma remains a barrier to Indigenous people seeking health care.
According to Stop TB Canada (the Canadian arm of a global TB advocacy forum), the most recent and complete TB-related data available in Canada is from 2017. While some data can be found on TB notifications from 2020, there is no detailed information publicly available on case outcomes, treatment adherence or even TB deaths.
A Public Health Agency of Canada report in 2018 found the average annual TB rate among Inuit was 290 times higher than for Canadian-born, non-Indigenous people. In addition, the incidence of TB in some Indigenous communities in Canada is higher than it is in some lower-middle-income countries such as Indonesia and Cambodia, where the worldwide TB burden is the worst.
In the statement of apology delivered by Prime Minister Justin Trudeau on behalf of the federal government, he characterized Canada’s management of TB in the past as deliberate, “destructive colonialism.” He further noted: “But an apology alone is not enough. We must also promise to do better. And although as a country we can’t change what’s already done, we can choose what we do next.”
So far, though, not much seems to have changed. Last November, Nunavut’s territorial government declared a TB outbreak. Media reports suggest federal funds have dried up and active TB screening through clinics has stopped, with staff diverted to responding to COVID. Stringent efforts are now urgently needed to ensure that the pandemic does not reverse the progress made in the belated fight to end TB.
We can learn from the Global South, where countries with high TB burdens have been innovative in community engagement for TB screening and treatment, and ensuring availability of point-of-care diagnostics. For example, India and Indonesia are using TB survivor networks for building awareness and advocacy.
TB programs in Nunavut still send TB patients to southern hospitals for treatment and bring health personnel from outside to do active screening, despite the federal government’s commitment in the apology “to finding community-owned, community-driven solutions.”
Identifying TB survivors in Nunavut as champions and involving them in community screening, contact tracing, and treatment monitoring could mitigate underlying stigma and mistrust. Digital innovations such as treatment monitoring through video calls and a survivor-support system will help in starting community-based treatment so that a patient does not need to leave home for treatment.
There are also new ways to diagnose TB early that can help limit the spread of the disease, again without significant added costs or personnel. Margaret Chan, former director general of the World Health Organization (WHO), notes: “Everyone with TB should have access to the innovative tools and services they need for rapid diagnosis, treatment and care. This is a matter of social justice, fundamental to our goal of universal health coverage.”
The federal government should consider new diagnostic technologies such as artificial intelligence integrated into digital x-rays and should add more portable molecular technologies and antigen-based skin tests (TBST), which is in the process of getting WHO approval. The devices used in this work are easy to carry and run on batteries, making them attractive to use in remote areas.
While better diagnostics can improve the current situation, the underlying social inequities that have allowed TB to persist need urgent attention. Food insecurity remains a constant challenge in Nunavut, and lack of nutritious food is a contributor to the spread of TB.
Again, there are lessons to learn from the Global South. A community-grown, peanut-based supplement, Plumpy’Nut, helped to improve nutrition of children in African countries. Similar approaches could be taken in Nunavut. Ensuring basic services such as safe running water and better housing is also badly needed. But in the meantime, some prevention strategies such as mask-wearing indoors and selfor community based-screening can be important tools to stop the spread of TB.
These initiatives will need financial resources and co-ordination between the federal and territorial governments, but they can help to tackle the double burden of TB and COVID.