(This article has been translated into French.)
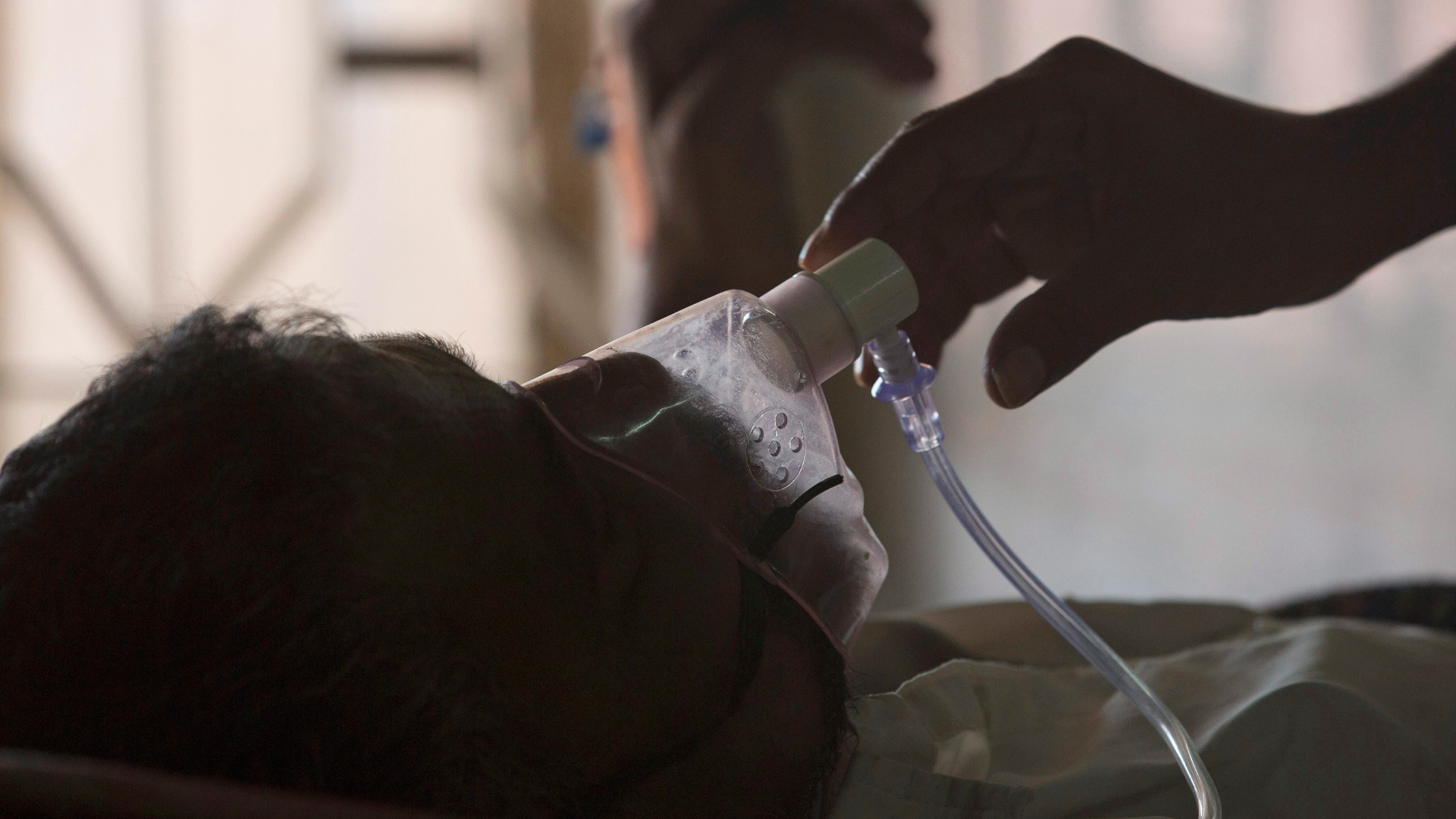
As we continue to face a global pandemic, it is timely to reflect on Canada’s leadership in global health. In particular, the unprecedented response to COVID-19 in terms of financial commitments by countries offers an important opportunity for comparison with another infectious disease: tuberculosis (TB). Prior to COVID-19, TB killed more people annually than any other infectious disease, causing 1.4 million deaths globally in 2019. Yet, TB has received deplorably little attention in terms of political engagement and financial investment. On World TB Day (March 24), we raise key calls to action for Canada with respect to ending TB at home and abroad.
Canada has built a strong global health leadership portfolio as a founding partner of both the Global Financing Facility (GFF) and the Global Fund. Canada is also a founding partner of TB REACH, which funds programs to improve TB case detection among the world’s most–affected communities. Canada is therefore well–positioned to take on an important role in the fight to end TB. However, for Canada to deliver on its commitments to global health and to TB elimination, it must do more.
Canada’s bold promises to global health are dimmed by the failure to deliver on them through adequate funding, and by the inadequacy of its response to domestic health inequities. TB is a clear example of the confluence of failures on both of these fronts. Although overall TB prevalence is low in Canada, the disease remains a significant concern in foreign-born and Indigenous communities, with the incidence of TB in Inuit communities being more than 290 times higher than in the non-Indigenous Canadian-born population.
That a disease which is both preventable and curable should still persist to this extent in Canada is indicative of unacceptable inequities. How can Canada claim to be a champion of global health if it continues to fall short of addressing such stark inequities within its own borders? The government of Canada has committed to eliminating TB across Inuit Nunangat by 2030. If it is to achieve this goal, it must back up the targets it has set with concrete political and financial investments.
There are a number of specific ways in which Canada can and should step up in the fight against TB at home and abroad. First, as a major funder of TB Reach, it is crucial that Canada continue its support for TB REACH. Given the significant disruption in TB services as a result of COVID-19, TB programs serving the most–affected communities urgently need renewed support.
Another opportunity for Canada is the Challenge Facility for Civil Society . This initiative provides funding to community and civil society organizations to promote a rightsand gender-equity-based TB response, aligning well with Canada’s feminist mandate for international aid. Strong financial investment in this initiative would therefore be a meaningful way for Canada to follow through on its goals and lend credibility to its priorities.
Canada must also hold itself and other countries accountable for progress made towards global TB-elimination targets, including those set at the 2018 United Nations General Assembly High-Level Meeting (UNHLM) on ending TB. Having global leaders come together for the first-ever meeting focused specifically on TB was a hopeful milestone. Unfortunately, there remains an immense gap between targets set by member states and progress towards achieving these targets. The Stop TB Partnership has issued urgent calls to action to close this gap. Canada must do its part by making the financial investments required to achieve TB targets and by increasing accountability for progress towards ending TB.
Furthermore, it is critical that Canada increase its investment in research and development. At the UNHLM on TB, a global annual target of US$2 billion in TB research funding was set, which could be met if countries invested their “fair share” in TB research, defined as dedicating at least 0.1 per cent of their total research spending to TB.
Canada failed to meet this target in 2019, spending only 76 per cent (US$19.3 million) of its fair share (US$25.3 million) on TB research (Figure 1). This places Canada behind the Philippines, New Zealand and the U.K., which met their fair–share targets, and behind the United States, which contributed 89 per cent of its fair share. Canada must step up its spending on R&D to contribute, at the very least, its fair share.
Lastly, if Canada answers this urgent call for increased investment in TB, it should also ensure that this investment is well-coordinated and strategically allocated. Its unco-ordinated resource allocation has previously fragmented and weakened the impact of Canada’s contributions to global health. Apart from simply contributing its fair share to R&D, specific areas of TB research would benefit from increased Canadian investment, particularly drug, vaccine and diagnostics research (see Figure 1).
It is alarming that these areas remain underfunded, given the outdated state of TB tools. To put this into context, the Bacille Calmette-Guérin (BCG) vaccine was developed 100 years ago, and despite its limited effectiveness, remains the only TB vaccine used today. In contrast, multiple effective COVID-19 vaccines were produced and rolled out within one year. This striking contrast highlights the fact that strong political engagement, backed by financial investment, is crucial for progress on developing new tools to prevent, detect and cure TB.
As a country with an encouraging track record of engagement and leadership in global health and in TB, but also a long history of neglect with respect to addressing TB in Indigenous communities within its own borders, Canada has both the means and the ethical imperative to step up in the fight against TB. With COVID-19 disruptions threatening to significantly reverse progress on TB, now more than ever, there needs to be a committed and co–ordinated Canadian response specific to tuberculosis. Most importantly, this response must be one that delivers on its promises through action and financial investment, and encourages global accountability for progress towards TB elimination.
The authors would like to thank Robyn Waite and Adam Houston at Stop TB Canada for their valuable feedback on this work.