If a Canadian wide-body jet were to crash because of maintenance problems, killing all 400 people on board, it would be seen as a national disaster and would occupy the news for weeks. If this happened each year, it would be unthinkable. But 400 is approximately the number of women in Canada who can be expected to die of breast cancer every year if screening for women in their 40s is cut back.
Yet a Canadian task force has once again concluded that doctors can afford to do less breast cancer screening for women in their 40s despite what is known: breast cancer is the most common cancer in North American women. It is also the second-deadliest cancer for women, with lung cancer being the biggest killer. One in six women who die of breast cancer are in their 40s.
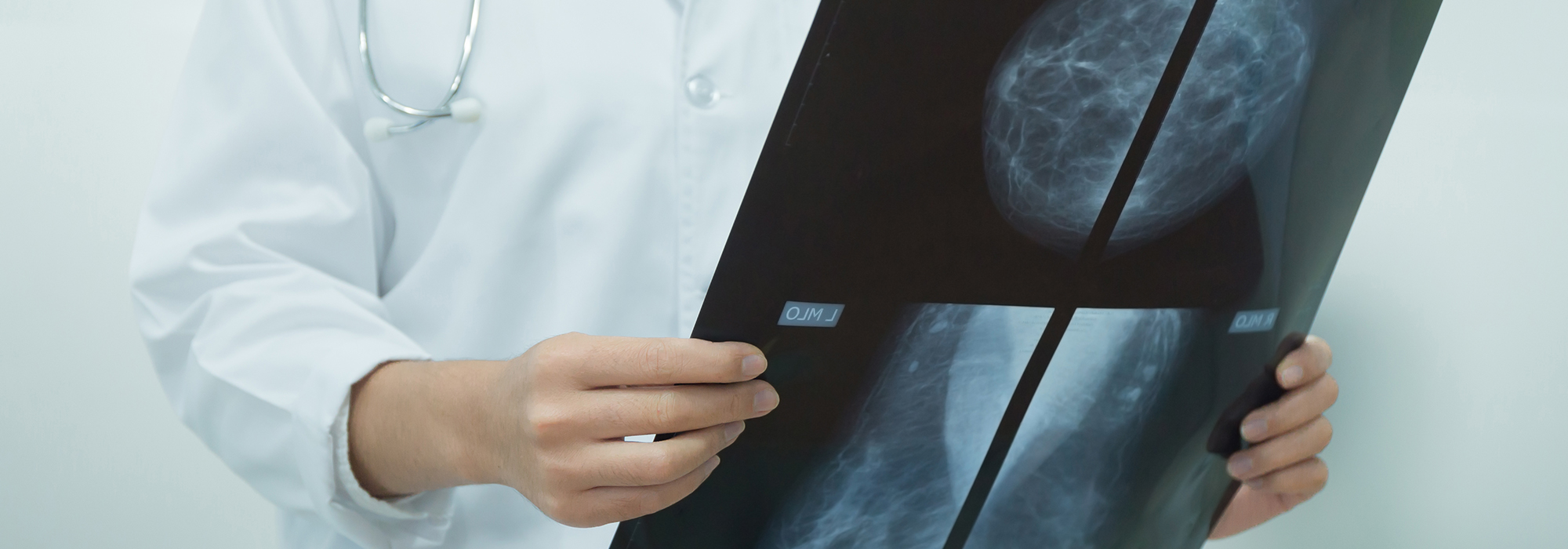
The only proven method of reducing breast cancer mortality is by earlier detection through regular imaging examinations using mammography. And ultrasound can be useful for supplementary screening for those women who have very dense breasts, where mammography is less accurate. It’s like using a sieve to sort stones from sand: many women are examined to find a cancer that will threaten a few.
The Canadian Task Force on Preventive Health Care is charged by the Public Health Agency of Canada to review scientific evidence and provide guidelines on interventions to improve the health of Canadians. In December 2018, the task force issued guidance on screening for breast cancer for women it describes as “not at increased risk.” The guidance is essentially unchanged from its highly criticized guidelines published in 2011. Again, the task force:
- recommended against screening with mammography for women aged 40 to 49;
- recommended screening with mammography every two to three years for women aged 50 to 74;
- recommended not using magnetic resonance imaging, tomosynthesis or ultrasound to screen for breast cancer in women not at increased risk; and
- recommended not performing clinical breast examinations to screen for breast cancer, nor advising women to do breast self-examinations to screen for breast cancer.
These recommendations are inconsistent with current scientific knowledge on the effectiveness, benefits and harms associated with breast cancer screening. Even the use of the term “not at increased risk” is problematic since the main risk factors for breast cancer are being a woman and being over 40.
The task force minimizes the impact of breast cancer in women in their 40s. Women of that age account for 16 percent of eventual breast cancer deaths, and in the tally of estimated years of life lost to breast cancer, women who are 40 to 49 years old when their cancer is detected account for 24 percent of those lost years. Further, the task force heavily implies that the benefits of screening are negated, even outweighed, by the harms, which include a risk of false-positive findings and overdiagnosis, where other less-lethal cancers are discovered. This is simply not the case.
By never expressing harms in a way that allows them to be compared against benefits, the recommendations are misleading and dangerous. They scare away women and their health providers from an intervention that can save lives and reduce morbidity and the costs of treating advanced disease.
How did the task force get it wrong?
The task force members are appointed as general methodologists, not experts in the area for which they are administering guidance. Importantly, they do not review the evidence directly but contract this responsibility to two external evidence review groups, at the Ottawa Hospital Research Institute and the Alberta Research Centre for Health Evidence, whose members also appear to lack subject expertise. This disconnect is dangerous, but the approach could have worked if careful attention were paid to the advice from external experts familiar with the strengths and limitations of breast cancer screening who have read the current research literature and understand some of the subtlety of the data. But this was not the case.
I was one of several people who expressed concern with the formulation of the guidelines, both before and after they were published. The federal Minister of Health and the Chief Public Health Officer responded by telling me the task force operates independently, at arm’s length from government. This is a good idea except when a group of appointed individuals lack the expertise to make a knowledgeable analysis and the judgment to heed the advice of experts. The results are likely to be disastrous.
The operating procedures for the task force appear to be reasonable. The problem seems to be that in 2011 and 2018, the task force began by choosing a policy — the goal being to reduce the amount of preventive health care. Then it cherry-picked evidence that supports that policy: that is, policy-based evidence.
This is poor governance and lack of oversight — an appointed group that has gone off the rails. This problem can be addressed only from above. The task force recommendations should be shelved until an external, competent, impartial review has been completed.
Benefits of screening
The rate of Canadian women dying of breast cancer has dropped by 44 percent since the late 1980s, when mammography screening began in Canada. The Canadian Cancer Society, the Public Health Agency of Canada and Statistics Canada attribute the drop to a combination of increased mammography screening and the use of more effective therapies after breast cancer surgery. (Details on page 20 of this report.)
The first evidence that demonstrated the life-saving potential of mammography screening came from randomized controlled trials conducted from the 1960s to the 1990s, which means some of the trials relied on imaging technologies that date back close to 60 years. Controlled randomized trials are conservative by design. They tend to underestimate benefits. Nevertheless, for women in their 40s, screening was credited with reducing deaths by 15 to 29 percent. For women between the ages of 50 and 59, the task force acknowledged, deaths dropped by 21 percent.
In the decades since the trials, there have been major improvements to the way in which mammography screening is performed and in the therapies for breast cancer. These include digital mammography (largely a Canadian invention), better surgical techniques and new, more targeted drugs. There is now a wealth of information available from modern studies of organized screening programs in Canada and other countries that shows mortality rates have dropped by 30 to 45 percent for women who choose to be screened.
There is also good evidence that when breast cancers are detected earlier through screening, there is less need for harsh, debilitating treatments such as mastectomy, axillary dissection (removal of lymph nodes in the armpit) and chemotherapy.
What the guidelines miss
The task force did not consider this evidence. Perhaps that was because the task force uses a Canadian-developed system for assessing evidence. The system, whose value I do not dispute, is called GRADE. It puts a high weight on randomized trials because they eliminate some of the bias inherent in other types of trials. But the results of a randomized trial are useful evidence only if the study addresses the relevant question: How effective is breast cancer screening today with modern technologies and methods and access to modern therapies?
Because the only randomized trial data were based on screening and therapy done in the ’70s, ’80s and ’90s — and not reflective of current practices — the task force could have looked at other modern data, which its operating procedures allowed it to do. It decided not to, ignoring the studies that suggest mortality dropped by 30 to 45 percent.
And by considering mortality rates only from the randomized controlled trials, the task force ignored a clear benefit to younger women when cancer is detected early: many more years of life and less aggressive therapy.
The task force requested but then ignored input from external experts in breast cancer and screening, as it did in 2011. In assessing any benefits of screening, it looked only at the randomized trials and their obsolete screening methods and treatments. But when it assessed the harms associated with screening, it was willing to consider any sort of data, even what it acknowledged to be poor-quality studies.
For example, the task force pointed to overdiagnosis as a major harm of screening younger women. Overdiagnosis refers to detecting cancers that would otherwise not be found — and would therefore not need to be treated — before a woman has died of some other disease.
Because other causes of death increase with age, overdiagnosis is more likely as older women are screened. The amount of overdiagnosis that occurs is notoriously difficult to quantify. The task force took its estimate from a highly criticized study that was not designed to measure this effect but produced the highest quantitative guess.
Given that it is usually impossible to distinguish “overdiagnosed” cancers from potentially lethal cancers, even under the microscope, choosing not to find them because some of them will be indolent – slow-growing and unlikely to become lethal – implies a willingness to miss an early chance to treat the killer cancers.
The task force also glossed over the need to incorporate ultrasounds into screenings for women with very dense breasts. Mammograms have limitations: they are less accurate for these women. But if women are informed that they have dense breasts and are referred for an ultrasound, this is a move toward more personalized medicine. Yet this sort of approach is explicitly rejected by the task force. There are no completed studies of screening with ultrasound in which the effect on breast cancer deaths is compared, although one is under way in Japan. But it has been demonstrated that ultrasound can find cancers missed with mammography in dense breasts.
The task force’s new recommendations suggest shared decision-making by a woman and her health care provider. They state that the decision to undergo screening is conditional on the value a woman places on possible benefits versus the harms from screening. I agree fully, but this requires accurate information, something the task force has not provided.
The task force should have presented a quantitative comparison of benefits versus harms using the accepted methodology of health quality analysis. That approach tracks the number of years of life saved because of screening, and it weights them by a number between 0 and 100 percent to reflect the quality of life during those years, yielding “quality-adjusted years of life” saved. Benefits of screening add quality-adjusted years of life; harms of screening reduce them. Such analyses have been published. The task force did not do such a comparison, despite my encouragement. Those analyses show that for women 40 and older, the quality-adjusted years of life gained from screening greatly outweigh the harms of screening.
Photo: shutterstock by Chompoo Suriyo
Do you have something to say about the article you just read? Be part of the Policy Options discussion, and send in your own submission. Here is a link on how to do it. | Souhaitez-vous réagir à cet article ? Joignez-vous aux débats d’Options politiques et soumettez-nous votre texte en suivant ces directives.