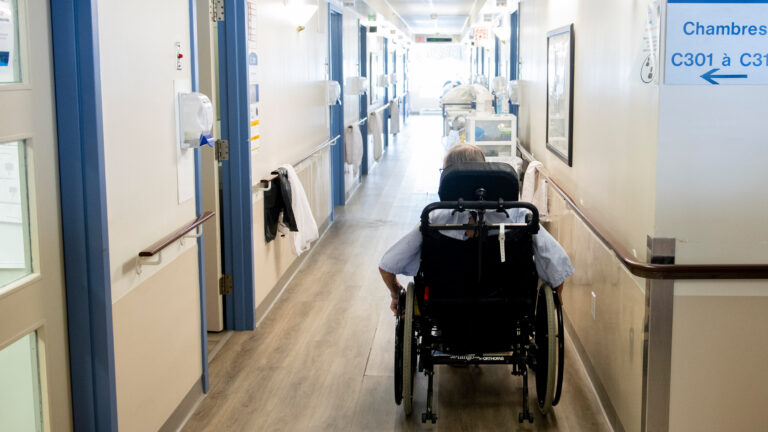
As a registered nurse working in a busy emergency department throughout this pandemic, I have witnessed first-hand the devastation of the COVID-19 virus on Canadians. However, it wasn’t until I began research into long-term care that I came to understand how policies intended to protect our most vulnerable ended up harming them.
It’s well-documented that the pandemic hit hardest our elderly and those caring for them. The number of deaths of long-term care residents has been devastating. But the unintended consequences of well-intentioned policies were what stood out in research I undertook with a group of researchers from the University of British Columbia led by Dr. Farinaz Havaei.
We need to learn from these consequences to reform pandemic management strategies for inevitable future pandemics. We also need to re-evaluate how long-term care policies are created – and why this process is overdue for a change.
Visitor policies for long-term care should consider what residents value
Seniors need trauma-informed services in long-term care homes
Cash-for-care benefits are key to reforming long-term care system
The pandemic has disproportionately affected the health of older adults worldwide, but Canada’s long-term care sector has been particularly hard-hit. In the first six months of the pandemic, nearly 70 per cent of COVID-19 deaths in Canada occurred in long-term care homes and retirement home residences -nearly double the international average. For decades, Canadian researchers and advocates have been raising the alarm about the poor care conditions and challenging work environments plaguing our long-term care sector. Experts largely agree that it is these existing deficiencies that allowed COVID-19 to grow into the tragedy that it has become.
When the B.C. government started to realize the detrimental effects of COVID-19 in long-term care homes, it adopted a series of pandemic management policies with the overarching goal to reduce harm to residents by reducing transmission of the virus.
Visitation was strictly limited, rigorous measures were enacted to prevent and control infection, and staff were limited to working at only one long-term care home rather than rotating among several, as was standard practice in the industry.
We looked at the impact these strategies had at one long-term care facility in Vancouver.
The policies curbed the spread of the virus at that facility, but they also substantially harmed residents, their families and the staff physically and mentally.
Strict visitation restrictions, especially at the beginning of the pandemic and during lockdowns, resulted in severe mental and physical distress for everyone, though they understood why the restrictions were vital. Restrictions were particularly difficulty for families of residents with cognitive impairment (e.g., with dementia or Alzheimer’s) because the families were prevented from providing care and advocacy for loved ones who might not be able to speak for themselves.
Restricting visitors also drastically altered the way families communicated with the care staff at the facility. “I can’t communicate basic things [that] I would co-ordinate with a care aide when I see them in the hallway,” one family member said. The physical and mental health of residents and families suffered.
Infection prevention and control policies also impacted the health of residents. Care slowed down because of the added time it would take to disinfect surfaces, and to put on and take off protective equipment. During lockdowns, residents were not allowed to leave their floors. For many, it felt like incarceration: “I wasn’t able to [go for a walk] and it did eventually really get to me,” one resident said. “I just really felt like a prisoner, and I was.”
The measures also added to the workload of the care home staff, taking a toll on their mental health. With staff restricted to working at no more than one long-term care home, overtime often had to be worked to fill gaps in staffing. Staff also faced an increased workload without families to provide substitute care.
On top of this, staff had to individualize engagement programs due to distancing requirements and had to find time to address the increased isolation, loneliness and decreased physical mobility of residents. Instead of organizing group activities, for example, recreational therapists could visit residents only individually in their rooms to, say, play cards. With the gym off-limits, residents had to wait for the physiotherapist for one-on-one sessions. These circumstances wore down care home staff (including leadership), and many described increasingly overwhelming feelings of emotional exhaustion, depression, and anxiety.
These are only a handful of examples of unintended consequences we uncovered at the facility we studied.
Of course, we know the policies were the right thing to do. We couldn’t let the virus ravage the care homes, and effective leadership during a crisis means taking quick and decisive action based on the available evidence. But we must learn from our mistakes and prepare better for the future to avoid further unnecessary harm to our most vulnerable.
So how do we do this? We have recommendations.
Residents, families and staff must be consulted early. They are directly affected by these policies and can help identify potential challenges and unintended consequences.
Their input can also help ensure policies go beyond a medicalized definition of health (how many residents contracted or died from the virus) and consider the important psychosocial elements of health, especially for those in the later years of life.
If the perspectives of residents and families had been incorporated early, increased workloads and their effect on care could have been acknowledged and accommodated within the policy. The willing volunteer community could have been put to good use instead of being locked out when it became clear that all hands on deck were needed.
Could down-payment federalism help kickstart reform in long-term care?
We can draw lessons from countries with strong long-term care systems
We might have realized that an additional staff member was necessary to co-ordinate communication between residents and families, and between care staff and families instead of asking an already overloaded staff to add the task to their days.
We might have realized that having a certified infection prevention and control practitioner in the facility was essential, and that all care homes should have one at all times. We might have realized that what the policy defines as “essential care” covers only physical health, whereas families consider a broader definition that includes mental and social health.
Including the perspectives of residents, family and staff in the creation of policy should become common practice.
Many care homes have resident councils and family councils made up of advocates more than willing to provide insights and be a part of the conversation. The more we normalize integrating these perspectives at all levels – in the research informing policy decisions, in policy implementation at the care home, in policy creation at the level of government – the easier it will be to incorporate their perspectives during times of crisis when quick, decisive action is required, and where the risk of harm can be minimized.