Some of us who couldn’t have distinguished between a ventilator and an air conditioning duct a month ago now find ourselves having opinions on supply chains and stockpiles of the device. The news is filled with stories about the likely shortage of ventilators in many communities as we hit the peak of the COVID-19 pandemic, and the worry is understandable. Because there is no proven therapy for the disease, ventilators are a last resort to keep desperately ill patients alive until their bodies can snuff out the virus.
But something has been lost in this preoccupation: how poor the outcomes are for COVID-19 patients once they are put on a ventilator. Most will likely die, and those who survive often have their health deeply compromised.
We have a death-denying culture. Our medical system throws all its energies and scientific power into saving lives, but we have neglected palliative care. And while we urge women to get mammograms and older adults to get colonoscopies, we do not work anywhere near as hard to encourage Canadians to acknowledge the reality that medicine has limitations. Right now, we should all be doing something that we have a tendency to put off to another day: talking to our loved ones about how we want to live and how we are prepared to die in the event of a personal health crisis. And health officials should be encouraging us to do so.
I began thinking about this in the context of COVID-19 the other day, when the well-known Canadian emergency physician Brian Goldman, who hosts the CBC Radio program White Coat, Black Art, tweeted that he would not want a ventilator.
Goldman’s determination to refuse a ventilator may come as a shock to you — as it did to many people who follow him on Twitter. As a medical practitioner, he understands what it means to go on a ventilator, but he is practically alone in trying to have a conversation with the rest of us about the hard facts of how this disease will end for tens of thousands of people around the world.
As COVID-19 takes over the respiratory system, in the most serious cases it leads to pneumonia. The filmy air sacs called alveoli, which normally capture oxygen in our lungs and keep us alive, become stiff with fluid, and the patient begins to suffocate. For the sickest patients, it is an agonizing condition, in which they are left literally gasping for air. Why would anyone choose not to use a ventilator at that point?
For one thing, hooking up the machine is extremely invasive. Patients are knocked out with sedatives and muscle-paralyzing drugs because the procedure is so aggressive that they could not tolerate it otherwise. Then a 10-inch tube is inserted into the lungs. The hope is that the oxygen will prevent the patient from suffocating to death before the body’s immune system is able to rally and overwhelm the virus, returning the patient to health.
But most people who go on a ventilator for COVID-19 will die without ever leaving the ICU — at least if current patterns hold. That’s another thing that doctors understand but many lay people do not. Because the pandemic has unfolded so quickly, it is impossible to give hard and fast numbers. However, one review conducted in China said that 86 percent of COVID-19 patients put on ventilators eventually died. In the UK, it seems that perhaps two-thirds of ventilated patients are dying.
For a small proportion of patients, the ventilator works: it keeps them alive for a few crucial days in which their body succeeds in fighting back. When the ventilator has been removed, they recuperate in short order.
But that is probably not typical. Writing in the New York Times, Kathryn Dreger, an internist and professor of medicine at Georgetown University, describes the more common outcome:
The amount of sedation needed for Covid-19 patients can cause profound complications, damaging muscles and nerves, making it hard for those who survive to walk, move or even think as well as they did before they became ill. Many spend most of their recovery time in a rehabilitation center, and older patients often never go home. They live out their days bed bound, at higher risk of recurrent infections, bed sores and trips back to the hospital.
When you understand all of that — when you know what doctors know — it is easier to understand Goldman’s decision. Although, to be clear, some doctors who replied to his tweet said that they would choose a ventilator if it were offered, even with their knowledge of the risks. They pointed out that it is difficult to know beforehand who may benefit and who may not.
But it is also crucial to note that this is not a purely medical decision. It is also a decision about personal values, which no doctor can prescribe for you. You may have to make the choice when you are in a very dire condition of body and mind. And the cruel reality of COVID-19 is that you will be cut off from loved ones — alone except for masked and gowned health workers who must keep their distance for their own safety. A spouse, a son or a daughter may have to make a decision for you over the phone. That is why it is so important to talk about this with them now.
As I have written about elsewhere, when my wife, Suzanne, was dying of breast cancer in 2016, neither she nor I was adequately prepared for the decisions we would have to make — or that I would have to make for her — at the end of her life.
My concern about this subject arises from a personal experience. As I have written about elsewhere, when my wife, Suzanne, was dying of breast cancer in 2016, neither she nor I was adequately prepared for the decisions we would have to make — or that I would have to make for her — at the end of her life. Since then, I have come to realize how important it is to engage in “advance care planning,” to ensure that those around you know your desires.
In recent years, some provinces, such as Quebec, have improved the legal structure permitting people to formally designate their preferences for critical decisions about their health, and there are online guides to help people start discussions with their families, such as this one for Ontario. But in this COVID-19 pandemic, I have not yet heard a single health official urge people to turn their minds to this task.
Like a lot of people, I put off the conversation in my own family. Some time ago, I legally designated my son Alex as my “substitute decision-maker” if I am too ill to make decisions on my own. However, we hadn’t really talked. He is just 21 and watched his mother die a little more than three years ago. I worried that it might be traumatizing to discuss the possibility that I, too, might get seriously ill or die. But I’ve recently realized that, as a 65-year-old man, I am on the cusp of the high-risk category for COVID-19. Do I want Alex to have to make the ventilator decision in a discussion with a doctor over the phone if I can’t express my wishes?
And so we began the conversation. I explained what I knew about the difficult outcomes for those who go on ventilators. I said that I put a higher value on the quality of my life than on its length. Good quality, for me, would mean having continued meaningful contact with Alex and his 17-year-old sister, Sophia. Perhaps also the ability to read and engage with the world of news and public affairs. I’d like to be able to watch the Winnipeg Jets play again — some day.
I told Alex to ask whether the doctors think there is a reasonable prospect of me recovering and coming off the ventilator in reasonably good health within a few days. The longer the time on a ventilator, the closer the association with poor outcomes.
This was the beginning of a conversation, not the end. The good news is that, like diving into a cool Canadian lake in summertime, it turns out that the hard part is getting in. When Sophia, whom I was continuing to protect, realized that her brother and I were having this conversation, she asked to be included. A wise move, because if Alex ever has to make life-and-death decisions for me, she will inevitably be part of the process.
There is another important question that has largely been overlooked: if someone doesn’t go on a ventilator when that is their only hope for life, how will they die?
Amit Arya, a prominent palliative care physician, and some colleagues recently wrote about palliative care in the pandemic for the Canadian Medical Association Journal. They describe what governments and the health care system must do to ensure the least possible suffering for those who will die. There is an urgent need for everything from the personal protective equipment we keep hearing about to medication kits to ease the ordeal of the dying. The fact that family won’t be there at the end may intensify their grief and sense of helplessness, and we need to think about how we can help them, too.
Our health authorities must explain much more clearly to the public what going on a ventilator really means. Patients and potential patients who do not understand the course of this disease cannot make informed decisions that will preserve their dignity and express their values.
I hope you will avoid COVID-19 by following all the official recommendations on handwashing and social or physical distancing. But you may get it anyway. Spare yourself and those close to you some avoidable anguish by doing advance care planning now. Even if it’s not needed soon, you will have launched a conversation that you probably should have got under way long ago.
This article is part of the The Coronavirus Pandemic: Canada’s Response special feature.
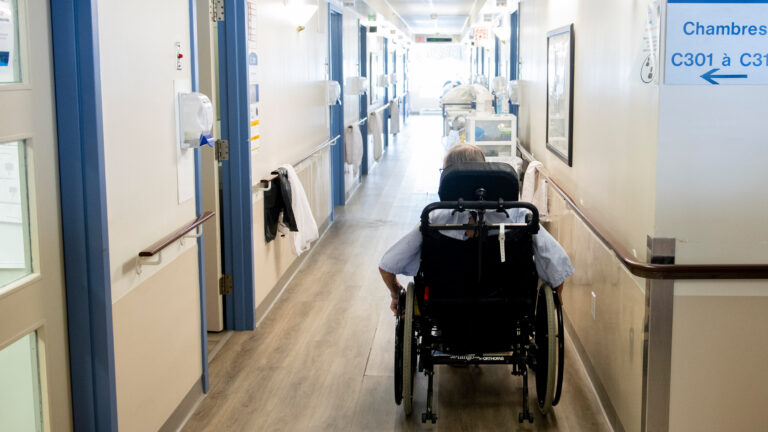
Photo: Shutterstock.com, by sfam_photo.