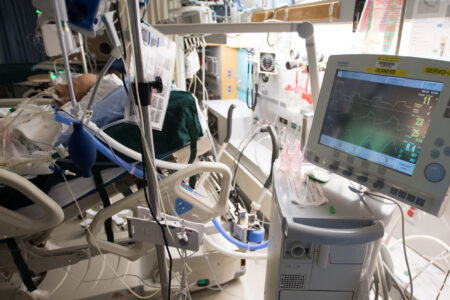
At a media briefing on April 3, Ontario government officials made public the data and projections they were using to build their strategy to minimize the threat posed by COVID-19. The briefing was described as an opportunity for the government to provide Ontarians with “full transparency.” It was also an opportunity for the government to justify its current population-wide lockdown strategy, which, as Premier Doug Ford described it, has ground daily life to a halt.
To justify its strategy, the government compared it with doing nothing, which it referred to as the “no intervention” option. In this scenario, the government estimated, there would have been 300,000 infections and 6,000 deaths by April 30, and 5 million infections and 100,000 deaths by the end of the pandemic. By adopting its lockdown strategy, the government estimated, it will have prevented 220,000 infections and saved 4,400 lives by April 30, and anywhere from 85,000 to 97,000 lives in the long run. According to the government’s more recent models, released April 20, its lockdown strategy is performing better than expected, having prevented an estimated 280,000 infections and saved hundreds more lives.
Assessing the current strategy against a no-intervention scenario is important, as it helps quantify, albeit imperfectly, the severity of the COVID-19 threat. The problem, however, is that it sets the bar too low and does not provide a robust enough test of the government’s approach. What we also need is a comparison of the government’s current lockdown strategy with other strategies that have been proposed to reduce mortality rates and burdens on the healthcare system. The decision to employ a population-wide lockdown strategy requires a high evidentiary standard; what’s more, public trust must be based on knowing that our governing institutions are thinking carefully through every possible policy option.
One alternative to a population-wide lockdown strategy involves implementing more targeted, age-sensitive measures that seek to reduce virus transmission rates among high-risk populations while keeping them normal among low-risk populations. In a March 16 paper, University of Pittsburgh’s Maria Chikina and Carnegie Mellon University’s Wesley Pegden describe a “heterogeneous mitigation” strategy that seeks to shift the distribution of infections toward age groups who are far less likely to require hospitalization and die from COVID-19, and away from older populations and individuals with pre-existing health conditions who are at a much higher risk:
To minimize hospital overcrowding, the goal is not to minimize the number of COVID-19 infections but instead the number of COVID-19 infections requiring hospitalization. Like overall mortalities, the COVID-19 hospitalization rate varies [by] orders of magnitude by age group, suggesting that to minimize the number of hospitalizations, we should seek to shift the age-profile of infections, rather than simply minimizing their total number.
In practice, as the virus circulates, a heterogeneous mitigation strategy involves ensuring individuals in high-risk groups stay home as much as possible, wear masks in public and avoid all non-essential travel. It also involves the temporary closure of nursing and retirement homes to all visitors and increased health and safety precautions inside these homes to prevent virus spread. Another important measure is increased vigilance among vulnerable individuals and their healthcare providers to catch early signs of pneumonia, a main cause of death among those who contract COVID-19. This approach, much like the Ontario lockdown strategy, would also involve a series of measures to scale up hospital capacity rapidly to address spikes in hospitalization. Unlike the government’s current strategy, however, heterogeneous mitigation would not impose severe restrictions on low-risk groups. Schools would remain open, as would most sectors of the economy. While measures would be in place to limit contact with vulnerable individuals as much as possible, this regime would otherwise allow low-risk groups to function as normal.
Which of these two approaches would result in fewer deaths and a faster return to relative normalcy? These questions may be difficult to answer but they are important to address.
In their modelling, Chikina and Pegden find that heterogeneous mitigation strategies result in reductions in mortality of 51 to 63 percent compared with doing nothing, and reductions in mortality of 24 to 63 percent compared with population-wide lockdowns. The difference is largely due to the fact that population-wide lockdowns delay the onset of herd immunity, thereby postponing deaths rather than preventing them. Once lockdown measures are relaxed but without herd immunity, a circulating virus can still do considerable damage to high-risk groups. Chikina and Pegden find that population-wide lockdown strategies “which end (even gradually) reduce the number of deaths only by 1% or so; as the mitigation efforts let up, we still see a full-scale epidemic, since almost none of the population has developed immunity to the virus.” By contrast, they suggest, a heterogeneous mitigation strategy prevents more deaths by allowing herd immunity to develop, so once vulnerable individuals re-enter society, the virus no longer poses a grave threat. Given that a vaccine appears to be at least 18 months away, the only way for near-term herd immunity to be acquired is through widespread infection and recovery.
The Ontario government may be right that its current strategy is the most effective way to suppress the virus that causes COVID-19. But, based on the projections presented, all we know is that it is better than doing nothing. The government should lay out which other policy options have been considered and examined, and how their performance would compare with the current strategy. Demonstrating that a strategy involving a population-wide lockdown is the best of all reasonable options would go a long way to helping the public commit to physical distancing measures over the long term. But if other strategies have been shown to be more effective and less costly, then it is important to know this now and pivot as quickly as possible to minimize the damage.
This article is part of the The Coronavirus Pandemic: Canada’s Response special feature.
Photo: A Toronto playground closed by the COVID-19 lockdown. Shutterstock.com, by auburnpetal