In our rapidly changing world, many potentially disease-causing micro-organisms are able to evolve and adapt at a rate that far exceeds our ability to develop new and effective drugs to combat them. Bacterial diseases are particularly notorious for this adaptive capacity, and the lack of new antibiotics to deal with multidrug-resistant strains of common bacteria such as E. coli and staphylococcus is generating concern among public health authorities worldwide. Other microbes showing a worrisome resistance to drugs include the bacteria that cause human tuberculosis and the protozoal parasite that causes malaria, plus many more.
Well before the discovery of antibiotics in the 14th century, the Black Death, an infamous pandemic of plague, killed more than 50 million people — over 50 percent of Europe’s population. The Black Death was caused by a bacterium transmitted to humans by the rat flea. It spread rapidly across overcrowded and rat-infested towns in Europe from 1346 to 1353. Chronicles and letters from the time describe the fear generated by the highly infectious disease.
Despite impressive progress since then in the development of our arsenal of chemical and management interventions, infectious diseases continue to be a significant worldwide source of human and animal illness and death. In modern times, our ability to fight back is being challenged by antimicrobial resistance (AMR), which results from natural and human-driven changes in the genetic makeup of micro-organisms. These genetic changes are brought about by exposure to chemical agents such as antibiotic drugs, other antimicrobials and disinfectants, as well as to some naturally occurring compounds. Unfortunately, the use, overuse, underuse and misuse of these antimicrobial agents in humans, animals and crops has contributed to the escalating global problem of AMR.
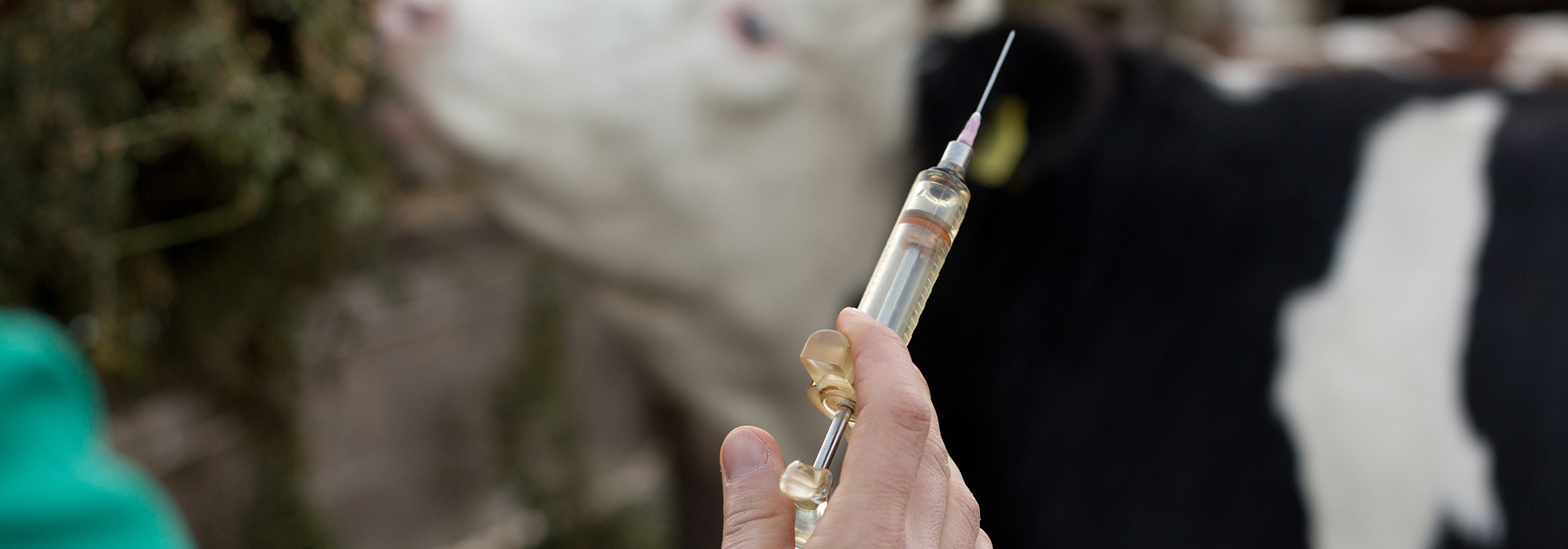
Antibiotics and antimicrobials are widely used in human medicine, livestock agriculture and aquaculture, and the ones used in agriculture and aquaculture are often similar to those used in human medicine. There is a growing concern that this use of antibiotics in humans and animals, including food-producing animals, can result in the strengthening and spread of antibiotic-resistant bacteria; the resistance genes can be passed from one microbe to another in human and animal populations and in the environment. How much microbes can change in a given time frame is hard to predict, because natural ecosystems are highly complex and the evolutionary pressures are variable.
The use, overuse, underuse and misuse of antimicrobial agents in humans, animals and crops has contributed to the global problem of antimicrobial resistance.
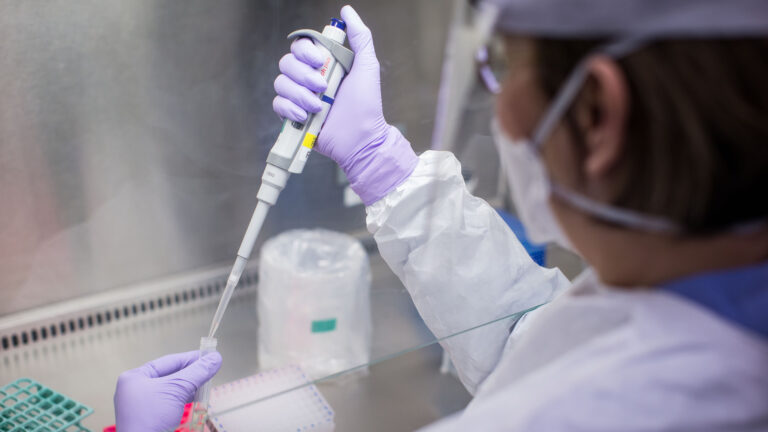
As existing antibiotics and other antimicrobial drugs rapidly lose their efficacy, there is not enough investment in developing replacement drugs or alternative approaches for the prevention and treatment of infectious diseases. Regulatory and financial barriers are blamed for the lack of research and development, especially on projects to reduce reliance on antibiotic use in livestock. The livestock sector needs new vaccines and more incentives for the development of innovative management options. We believe that neglecting these issues is short-sighted. More must be done to promote research and development in this area, especially for zoonotic diseases (those that are shared by humans and animals). Similarly, greater investment is vital to develop new diagnostics to detect and characterize drug-resistant micro-organisms. If we fail to focus attention and resources on AMR, many of the tools we currently have to control disease in humans and animals may become ineffective within the next few decades.
Although the speed of genetic change is uncertain, the threat from AMR is increasing, and urgent action is needed. Experts agree that all sectors (human medicine, veterinary medicine, public health, agriculture) and the relevant regulatory agencies need to work together to improve the stewardship of drugs, antimicrobials, disinfectants and other chemical agents currently available to treat or prevent infectious diseases. It is a highly complex challenge that requires collective and comprehensive action on a global scale. The World Health Organization (WHO) developed a draft global action plan in 2015 to combat AMR. Each member country should have a national action plan in place by the 70th World Health Assembly, which will be held in Geneva at the end of this month.
A number of national and international AMR surveillance programs are already in place to assess the problem, and many governments have developed AMR action plans. Here in Canada, the Public Health Agency of Canada (in collaboration with Health Canada, the Canadian Food Inspection Agency, the Canadian Institutes for Health Research, Agriculture and Agri-Food Canada, the National Research Council Canada and Industry Canada) published in 2015 a Federal Action Plan on Antimicrobial Resistance and Use in Canada. The document outlines the need for government leadership with enhanced surveillance for AMR, better stewardship for the prudent use of antibiotics and a targeted approach to encourage research and innovation. Guidelines and recommendations are being developed to implement the plan, and food and drug regulations are being updated.
With changing global demographics and growing international trade and travel, no country should be considered in isolation. Emerging and re-emerging infectious diseases do not respect national borders, and micro-organisms are readily carried around the globe on animate and inanimate objects. It is important to understand how highly interconnected everything is: actions — and lack of action — in a far corner of Africa or Eurasia can affect diseases that threaten health here in Canada, and vice versa.
Many good initiatives are under way at local, national and global levels to address AMR, but what is also needed is enhanced vigilance and an ongoing commitment from a wide range of stakeholders, including veterinarians, medical doctors, farmers and the general public. World Antibiotic Awareness Week (November 13-19, 2017) aims to raise awareness and educate the public about antibiotic use and how everyone can play a part in efforts against AMR. Simple actions such as improving hygiene, hand washing and taking the full course of antibiotics when prescribed can help prevent infectious illness and prolong the efficacy of our current antibiotics. We all need to take responsibility for our own health, as well as the health of the environment and all the living creatures with whom we share the planet.
This article is part of the Canadian Agriculture at the Cutting Edge special feature.
Photo: Shutterstock/Budimir Jevtic
Do you have something to say about the article you just read? Be part of the Policy Options discussion, and send in your own submission. Here is a link on how to do it. | Souhaitez-vous réagir à cet article ? Joignez-vous aux débats d’Options politiques et soumettez-nous votre texte en suivant ces directives.