It is time we talked about the grief.
First, the sheer volume of it. There have been more than 5400 deaths from COVID-19 in Canada right now. But we know that is an undercount. And we know that the number will grow long after this first peak is passed.
We know also that yet more people are dying out of fear: for example, they have been slow getting to the emergency room for a heart condition. We know that more people are going to die, or die sooner because of postponed surgery, chemotherapy or radiation.
Except for the most luckless among the dead, each individual leaves behind someone grieving deeply for their loss, and most will leave behind three, four, five, perhaps many more.
Second, it is the character of that grief. Many of those who die from COVID-19 do so in a hospital or care home cut off from their loved ones. If they have a chance to say goodbye, it may be on a phone or tablet held briefly aloft by a harried health care worker. Things that should have been said will remain unsaid. If someone is holding their hand at the moment they pass, it will be a nurse, wearing a mask and gloves. The people who love them and would have wanted to be there are instead at home waiting for the phone to ring.
In recent years, we have begun as a society to take matters of mental health much more seriously, if not yet seriously enough. It is not widely known, however, that grief or bereavement are not included in either public or charitable programs for mental health, including in this pandemic.
That is why the Canadian Virtual Hospice, a pioneer in dealing with issues of life-ending illness online, has convened the Canadian Grief Alliance. This is a coalition of experts, including psychiatrists, psychologists, social workers and therapists, that has come together to ask all levels of government to turn their minds to this issue urgently in the context of COVID-19.
What is grief? It is the normal human reaction to profound loss. Many of us have suffered it in our lives. If we are otherwise well situated, it eventually goes away -or to be more precise, it never goes away but it retreats to a place where it no longer prevents us from functioning at work, at school, or in our social lives.
Because grief is a “normal” response to loss that many of us survive with just the support of family and friends, the mental health system has not paid it much attention. But there is nothing normal about what is happening in the world today. Individually, we need to reach out to those we know are suffering. Collectively we need to talk.
What the research tells us about grief is that if it is complicated, it may become prolonged, entrenched, perhaps even transformed into depression, PTSD, or thoughts of suicide. Everywhere in this pandemic, we see complications.
It is not normal to be unable to say goodbye to a loved one. In many cases, families are isolated from their loved ones for weeks before they die. And for “normal” grief to occur, most of us need ritual. The funeral. The service. The visiting family bustling around the home, making sure everyone is fed. Today, at best, we have an hour or so on Zoom. This loss of ritual affects not just the bereaved of those with COVID-19. It affects the commemoration of every one of the 25,000 or so people who would have died in any other month. It affects the parents of a young child who has died of cancer and it affects the neighbours of those who died in the Nova Scotia shootings.
For some of the bereaved this grief-in-isolation is also occurring when they have just lost a job, or fear that they are about to do so. Some are struggling with their own delayed medical treatment or cut off from mental health supports. Some are just achingly lonely at an already lonely time.
In the next few weeks and months, the Alliance believes we must create free and accessible services for the grieving, online, on the phone, through services such as FaceTime and Zoom, and eventually, again in person. What people crave when they are grieving is connection, often with those who have been through something similar. It can help to put a name on their feelings and understand that with the help of others they can get through a difficult time. The needs are especially great among underserved populations such as Indigenous peoples, the homeless, people living in rural and remote areas, immigrants, refugees and the young.
We also need to make more people aware of the resources that already exist, such as MyGrief.ca and KidsGrief.ca, where people can get information about the grieving process and have their questions answered.
We must recognize also that this pandemic of grief will affect more than just those whose family members or loved ones die during this strange time. Imagine living in a long-term care home where a roommate or someone you saw each day at breakfast has died of the disease. Imagine being the custodian mopping up room after room, wiping them down with disinfectant, because the people you had known there have died and someone else needs the bed.
The general public may not be fully aware that among health care workers, there was also something of a mental health crisis before this pandemic. Physicians are said to have a suicide rate double that of the general population. So, spare a thought if you have not already, for the respiratory therapists, nurses and doctors fighting this virus.
COVID-19 is an especially intractable disease right now. There isn’t a lot that can be done. People whose life work is to heal the sick may feel helpless. Those who work in the ICU know that many, perhaps most, who are rolled into their unit will not roll out alive. Many of those health care workers are isolated from own families when they go home, for fear of spreading the disease.
There is an urgent need to provide grief supports now for these frontline workers, who are apt to feel they need to “suck it up” for the good of their patients and the community. But this pandemic is not going away in the next few weeks. It will be with us in all likelihood for a while. Sucking it up is not a solution for the long haul. We have a duty not just to alleviate the suffering of these frontline workers, but also an interest in keeping them healthy.
The Alliance believes we should take the next few months to consult and develop a national strategy including all levels of government, the public, private and charitable sectors. There needs to be an investment in research as well as in services.
The goal is not just to alleviate human suffering, but to allow workers to be their most productive, students to fulfill their potential, and to allow us collectively to avoid the financial costs that will come if grief becomes mental illness.
Each of us, of course, has a responsibility in our own lives to do what we can to comfort the bereaved. But the scale of the suffering is such that we must also act collectively.
This article is part of the The Coronavirus Pandemic: Canada’s Response special feature.
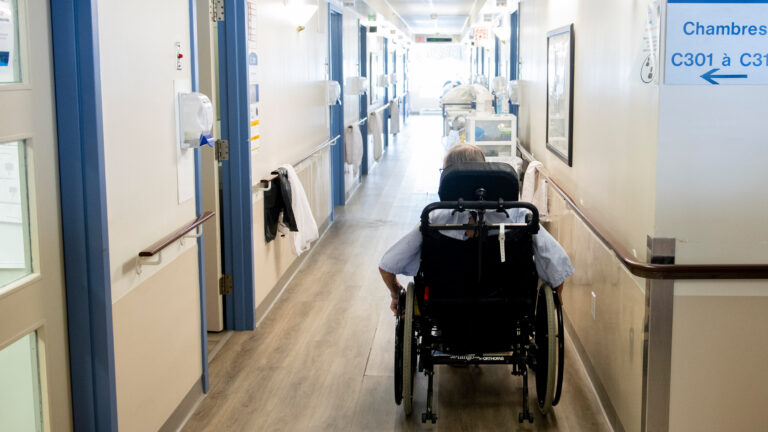
Photo: Shutterstock.com, by Elena Dijour