(This article has been translated into French.)
A few years ago, a pregnant friend who went through successful in-vitro fertilization (IVF) called me late at night, sobbing. She felt her baby kicking, and her mind wandered to her remaining embryos, stored for the time being in the freezer of the fertility clinic. She was overwhelmed by a sense of guilt. “I know I’m being completely irrational,” she said, “but I can’t stop thinking that they are cold, and I’m not there to protect them.”
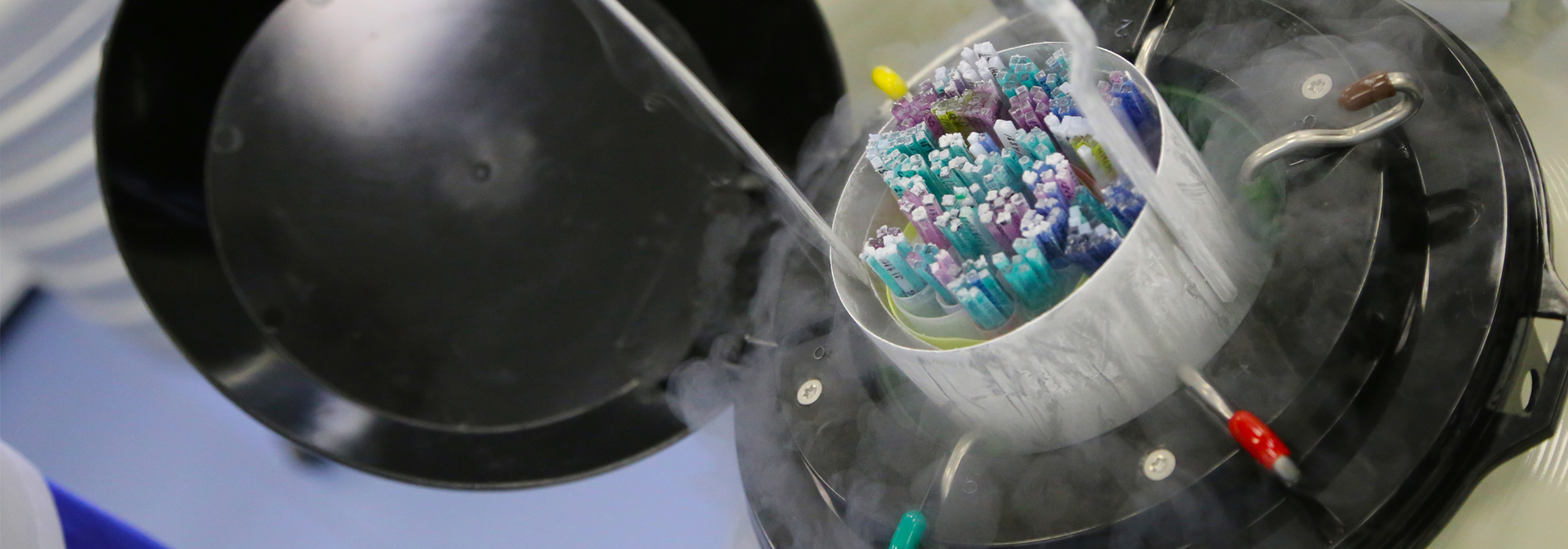
Countless frozen human embryos are sitting in freezers around the world today, and their number is growing. A cycle of IVF typically produces more embryos than can be implanted, and these excess embryos are usually frozen for possible future use. Unless the couple (or woman) returns to use them to have more children, or donates them (for research, training or to another woman/couple), these “leftover” embryos can sit in the freezer indefinitely.
These frozen microscopic entities can have immeasurable emotional value and profound symbolic meaning for those who created them. They are often seen as future children and potential siblings. They can represent the only hope for a genetically related child for those who preserved them prior to cancer treatment or injury. They are symbols of the tremendous time, economic sacrifice and physiological difficulty required to produce them. For many, they hold some moral status. For some – namely those who think life begins at conception – they can have the full moral status of a human being. Biologically, they are just a tiny group of cells, but for those who care about them, they are much more.
From a biological perspective, we do not know how many years they can survive on ice. In 2017, a baby girl was born from an embryo that was frozen 24 years earlier, the “oldest” embryo known to result in a live birth to date. It is possible that this could also happen after 100 years. We simply don’t know because we haven’t tried.
Experience in Canada and elsewhere suggests several things can go terribly wrong, jeopardizing the future of such frozen embryos. Yet despite these concerns, Canada has done a surprisingly poor job regulating it. Considering the symbolic importance of frozen embryos, clear policies should ensure they are well-protected.
First, the physical survival of frozen embryos can be threatened by natural disasters, emergencies and freezer malfunctions. In 2012, when superstorm Sandy hit New York, doctors and nurses at a Manhattan fertility clinic raced against time hoisting drums of fuel up darkened stairwells to feed a failing generator and saved numerous frozen embryos, later naming the resulting babies “Sandy saves.” Earlier this year, 4,000 frozen eggs and embryos were lost at a Cleveland fertility clinic due to unmonitored temperature fluctuation of a storage tank. Couples affected said they felt crushed and betrayed, one patient saying: “You shouldn’t go into IVF wondering, ‘Is the storage tank going to fail? Is there a chance I’m going to lose our eggs and embryos…?'”
While not all circumstances can be foreseen, careful planning can mitigate some. Clinical guidelines (such as those issued on various topics by the Canadian Fertility and Andrology Society) should require that freezers be backed up by generators, that extra safety precautions are applied, and that there are emergency plans in place in case of natural disaster. In addition, counseling and consent prior to storage of embryos should clearly outline the limits of such protections, since current federal consent requirements do not address this issue. Awareness of such limits might lead some people with embryos in storage to keep their them in two locations to minimize the risk of losing them all.
Second, while embryos are often created by a loving couple who share the dream of having a child together, things can change. Cases of separation or divorce have notoriously led to fierce disagreement over the fate of frozen embryos. The most mediatized recent case involved the actress Sofia Vergara and her ex-fiancé Nick Loeb. He wanted to take control of embryos they conceived together and implant them in a surrogate mother. When she objected, he not only sued as their progenitor but later re-filed, with the embryos (that he named Emma and Isabella) as plaintiffs, arguing that they have a right to live. Sounds crazy? Perhaps, but in certain jurisdictions it’s a trick that might work.
Here again, while not all scenarios can be predicted, many can. Couples should receive thorough counselling so that they have the opportunity to consider future eventualities such as change of heart, separation, divorce or loss of capacity by one partner. Since the regulations require that consent be given by a person “after receiving information meant to help the person understand his or her choices,” clearer guidance on the nature of counseling is greatly needed. Granted, many couples invested in a joint baby-project are not inclined to discuss these unfortunate scenarios. But such discussions could prove to be critically important later on.
Third, tragic circumstances can lead to the death of one partner and raise the issue of post-mortem reproduction. Quebec, for example, includes this possibility in the consent form that couples must sign prior to IVF. A study of 495 signed consent forms we published in 2014 showed that 73.5 percent of men and 61.8 percent of women agreed to post-mortem reproductive use of frozen embryos by their surviving partner. But follow-up in-depth interviews showed that some did not understand what they had agreed to, or were falsely convinced that they had actually refused.
Consent that is given under circumstances of informational overload and confusion is uninformed and worthless. Bringing a child into the world after the death of one genetic parent is an ethically complex issue. But this complexity makes it even more important to ensure that, at the very least, the wishes of the deceased partner are clear. Here again, appropriate counseling is critical, though it is not currently provided.
Finally, in some cases, those who created the embryos stop paying storage fees and simply disappear. Clinics’ attempts to reach them fail, and the embryos left behind are dubbed “abandoned.” Fertility clinics in Canada are allowed to destroy frozen embryos if storage fees are not paid, but this is a morally burdensome decision, and some clinics prefer to shoulder the cost of continuing to store the embryos than to make a potential mistake. Appropriate counseling of IVF users about what will happen if they abandon their embryos is needed so that their consent is truly informed. Clear time limits on embryo storage, telling clinics how many years they can (or should) keep “abandoned embryos,” is also needed and is an approach taken by other jurisdictions.
Clear and detailed policies and guidelines can greatly assist in the prevention or resolution of many ethical and legal conflicts related to the fate of frozen embryos. It is critical to ascertain the responsibilities of clinics and users in advance. But it is also important to remember that at the time of IVF, people can be overwhelmed with large amounts of information related to the process itself.
Potential issues such as the accidental loss of the embryos, conflict between partners, the death of a partner or the abandonment of embryos are not likely top of mind when people freeze their embryos. Appropriate counseling is thus of paramount importance to ensure consent is informed and addresses nuances and possible scenarios. These potential lives on ice deserve to be taken seriously.
This article is part of the Addressing the Gaps in Canada’s Assisted Reproduction Policy special feature.
Shutterstock by Ekaterina Georgievskaia
Do you have something to say about the article you just read? Be part of the Policy Options discussion, and send in your own submission. Here is a link on how to do it. | Souhaitez-vous réagir à cet article ? Joignez-vous aux débats d’Options politiques et soumettez-nous votre texte en suivant ces directives.