Legalization of cannabis in Canada has potential benefits — lower criminal justice costs, new government and private revenue sources — but we must also recognize the public health costs of cannabis use. It’s vital to ensure that governments at all levels use the available policy levers to reduce these costs.
Costs of cannabis use
According to the Canadian Substance Use Costs and Harms study, cannabis accounted for 7 percent of the cost of substance use in Canada in 2014: $2.8 billion out of $38.4 billion. This figure includes costs associated with health care for those with health conditions related to cannabis use (such as cannabis dependence, injury from driving accidents due to cannabis impairment and lung cancer) as well as lost productivity due to these health conditions. It also includes criminal justice costs for policing, incarceration and court proceedings associated with cannabis-related crimes.
More than 1 in 10 Canadians (12.3 percent) over the age of 15 reported using cannabis in the past year in 2015, an increase from figures for 2013. A proportion of those who consume cannabis — 6.8 percent, according to the 2012 Canadian Community Health Survey — will experience problematic use or dependence. According to data (not yet published) from the Canadian Institute for Health Information, the number of Canadians hospitalized to treat cannabis-related substance use disorders more than doubled, from 2.7 to 6.2 per 100,000, between 2006 and 2015, and health care costs due to cannabis use increased by 28 percent between 2007 and 2014.
Cannabis use impairs drivers’ ability to operate motor vehicles safely. In 2012, traffic collisions attributable to cannabis use had an estimated cost of more than $1.09 billion, including 75 deaths and 4,407 injuries. Statistics Canada’s National Cannabis Survey, conducted between May and June 2018, found that 14 percent of people who use cannabis overall, and 27 percent of those who use cannabis daily or almost daily, reported driving within two hours of consuming cannabis.
Although these numbers are worrying, we must recognize that the economic burden of cannabis is far less than that of two currently legal psychoactive substances, alcohol and tobacco. In 2014, only 2 percent of health care costs for substance use, amounting to $208 million, was cannabis-related, compared with alcohol at $4.2 billion (38 percent) and tobacco at $5.9 billion (53 percent). The cannabis figures are no cause for complacency, because the harms associated with alcohol and tobacco emphasize the need to make public health a priority when regulating psychoactive substances.
Improving what we know
Decades of research have established reliable relationships between increased consumption of alcohol and tobacco, increased harms and increased health system costs. We do not yet have comparable knowledge for cannabis. The illegal status of cannabis has complicated research by restricting access, making ethics approvals difficult and casting doubt on the reliability of self-reporting. Much of the existing evidence on health impacts is based on product potencies and formats that do not reflect the current illegal market or the anticipated legal market. The knowledge base is improving as recent research on the medical use of cannabis has advanced our clinical understanding of both its harms and its benefits.
Legalization will open the door to further research on how to minimize harms and maximize benefits. For example, studies are under way to examine the relationship between cannabis use and the use of other substances such as opioids and alcohol. If significant numbers of people opt to use cannabis instead of other substances, this “substitution effect” could have public health benefits. But if we see an increase in cannabis use and no corresponding decrease in other substance use, the increase in harms could have significant costs.
Public health policy levers
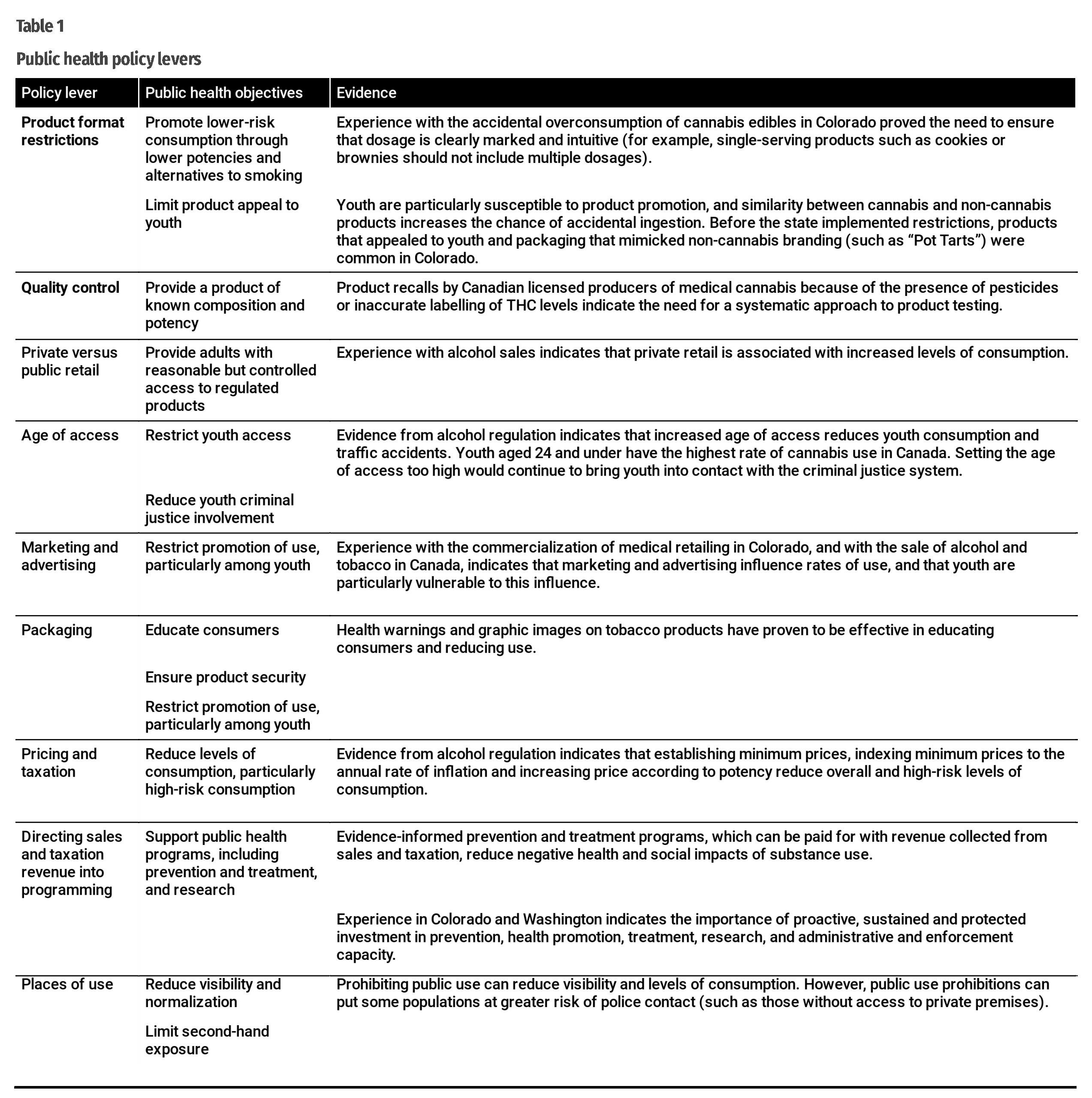
Looking at the experience of jurisdictions that have already legalized cannabis and Canadian experience with the regulation of alcohol and tobacco, we can identify key policy levers that could reduce the public health impacts of cannabis use. Table 1 summarizes these policy levers, the objectives they are intended to achieve and some of the key evidence we have about their application. These levers have been interpreted differently in provincial and territorial cannabis regulations. For example, Alberta and Quebec are the only two provinces that have set the age of access at 18 rather than 19; and Nova Scotia is the only province that will sell both cannabis and alcohol from the same retail location. These and other variations will provide an opportunity to evaluate and learn from different approaches.
Moving forward
Canada has the chance to provide international leadership for a public health approach to cannabis. Realizing that opportunity means applying the available policy levers based on the evidence we currently have and calibrating them according to the evidence we gather after legalization. It means prioritizing public health over revenue generation, something we have not done well with alcohol. It means providing Canadians the information they need to make responsible, educated decisions about cannabis use by scaling up prevention and education initiatives and promoting guidelines for lower-risk cannabis use. It means equipping our health system to support those who encounter problems with use by addressing existing gaps in tools and information for primary care providers. It means improving and increasing specialized services for youth, Indigenous people and those who live in rural or remote communities. Protecting public health also involves protecting public safety, which includes improving education and enforcement capacity to reduce cannabis-impaired driving.
Cannabis has been the most commonly used illegal drug in Canada and internationally for many years. Legalization provides an opportunity to reduce the many costs of a criminal justice approach. It also comes with the risk of increasing public health costs if we fail to make good use of the policy levers available at all levels of government by investing in effective prevention, education and treatment programs. Many countries are looking to Canada to inform their own decisions about cannabis regulation. We have an opportunity to demonstrate that legalization does not have to lead to commercialization. What’s more, it can be an opportunity to reduce public health costs by opening the door to a better understanding of the risks and benefits of use, and to honest dialogue with youth and other consumers about reducing those risks.
This article is part of The Economics of Canadian Cannabis special feature.
Photo: A Canadian flag with a marijuana leaf on it flies during a 4/20 rally on Parliament Hill in Ottawa, on April 20, 2017. THE CANADIAN PRESS/Sean Kilpatrick
Do you have something to say about the article you just read? Be part of the Policy Options discussion, and send in your own submission. Here is a link on how to do it. | Souhaitez-vous réagir à cet article ? Joignez-vous aux débats d’Options politiques et soumettez-nous votre texte en suivant ces directives.