Listen to governments around the world and the COVID-19 strategy is remarkably similar: muddle our way through until we have vaccinated enough of the population and the pandemic can be declared to be over. What “enough” of the population means is still up for debate with an amount of herd immunity (which may be as high as 85 per cent or more) or maybe everyone who can be safely vaccinated. But the overriding premise of this strategy is that the pandemic has an end; that is, a point in time that we will mark the return to normality.
If pushed, we all know that there won’t be a VE-Day like at the end of a war, but there is a belief that this is something that will be over. It is that premise that we need to challenge and put behind us. In all likelihood, COVID-19 will never be over. It will continue and morph into a seasonal illness. In other words, it will become endemic.
This is the consensus view among epidemiologists. Jesse Bloom, a virologist at the Fred Hutchinson Cancer Research Center in Seattle told The Atlantic, for COVID-19, “the optimistic future is that there are still infections but they are less frequent than now … and most infected people have something more resembling a cold than a life-threatening infection.” This is what happened with the pandemic of 1918-20, which eventually morphed into the seasonal flu. This is also the pattern for the four coronaviruses that currently circulate and that are responsible for the common cold. In other words, these viruses are endemic, and we learn to live with them.
Realizing that COVID-19 might not end should not change our current vaccination strategy. We still want to vaccinate as quickly as possible. But without an end, vaccination doesn’t buy as much as we have been hoping for. Vaccination won’t give us a solution but instead will prepare the population for ongoing cycles. The hope is that, in particular, older members of the population will continue to have immunity while younger members will gain immunity largely from future exposure.
There are, however, many unknowns. We do not know how long vaccine immunity will last. New variants – and we have already seen this – could “get around” current vaccines and, thus, like flu vaccines, variants may be an ongoing part of our lives. We also don’t know how harmful future COVID-like diseases will be. With influenza, new strains are still harmful and rank high on the list of causes of fatalities.
The problem with acting as if the pandemic has an end and is likely not to be ongoing is that we are unprepared for the latter. Part of this is being unprepared psychologically, and it is hard to find a psychologist who will argue that denial is a good mental health strategy for anyone. But the other part is that we are not doing other things that we need to do.
Two come to the fore. First, we need to invest heavily in treatments. There are now (compared to a year ago) effective treatments for COVID-19 but the fatality and hospitalization rates for COVID-19 are still extremely high relative to other endemic viruses. We put our money and energy into vaccines but there needs to be a similar big push to develop new treatments. Some of these may come from re-purposed treatments that currently face regulatory and other disincentives that harm their development.
Second, we need to have a proper surveillance infrastructure. At the beginning of an endemic period (in the first few years after a pandemic is officially over but the virus still circulates), outbreaks come periodically and could overwhelm our hospital capacity. That means we have to continue to “flatten the curve,” a phrase that seems so early 2020 now but is still relevant and will be more so over the next few years. We want to do that without lockdowns. That means that we need an infrastructure that can easily scale up and scale down testing and screening as the case may be. This is something I outline in my recent book on the pandemic. We do not yet have that infrastructure to deal with screening at scale although it is in development. We will likely need it.
It is understandable to hope for an end to a global calamity. But we tend to be over-optimistic about how quickly things can be resolved and whether they can be resolved at all. (Most people, for example, thought the First World War would be over in a few months.) Instead, we need to come to grips with the likelihood that this will be an ongoing problem we need to prepare for. The first step is for our politicians and public health officials to publicly communicate that this is the scenario we are facing.
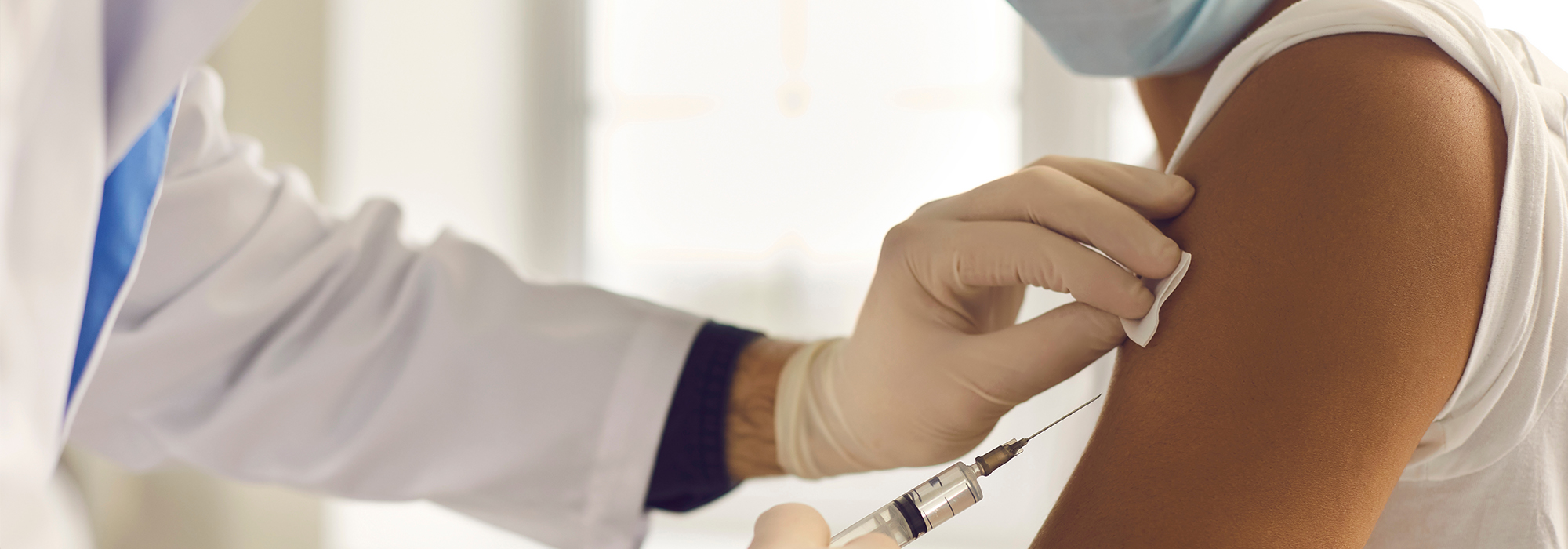
Photo: Shutterstock.com, by Studio Romantic.