The COVID-19 pandemic has painfully illustrated what people who use drugs have long known: that the current overdose crisis is more of a “drug poisoning crisis,” and that until a regulated supply of opioids, stimulants, and other substances becomes available, people who use drugs will continue to face extraordinary risk – and many will die.
British Columbia has seen record numbers of overdose fatalities in May, June and July 2020, and the City of Toronto experienced 27 opioid overdose deaths in July alone. This follows years of preventable deaths – over 15,000 opioid-related deaths in Canada between 2016-2019 – traceable most notably to the toxic drug supply tainted with fentanyl and other deadly fentanyl analogues.
Importantly, it is no longer just people who use drugs and their allies calling for the implementation of safe supply programs and scalability of the existing programs. Public officials and organizations including Vancouver’s City Council, British Columbia’s Provincial Health Officer, Dr. Bonnie Henry, and Chief Medical Officer of Vancouver Coastal Health, Dr. Patricia Daly, have also emphasized that a shift away from criminalization of drug use to a public health approach, centred on a regulated supply of substances, is critical to reducing the harms created by a contaminated drug supply. Even the Canadian Association of Chiefs of Police has endorsed decriminalization of personal drug use in a recent report favouring treating substance use with a public health approach.
However, as support for safe supply grows, and as research on how best to deliver safe supply and the piloting of safe supply initiatives (already established in sites across Canada) proliferate, it is critical that the people who are trying to access safe supply be recognized as leaders and experts on the meaning, delivery and sustainability of safe supply. If people who use drugs are not meaningfully involved, the quality of the research and its long-term impact upon policy and service delivery – the sustainability of safe supply – is likely to suffer.
Further, when people who use drugs are not engaged in safe-supply research and policy-making – or are involved only in a tokenistic way – it adds to and deepens the structural challenges of marginalization, isolation, and stigma, which are all too familiar to the drug-using community. What is experienced first-hand as safe is likely to be influenced by race, gender, socio-economic status and other social circumstances that affect how safe supply is delivered. It is also likely to depend on whether the design of so-called safe supply reflects and honours the agency of people who use drugs, and whether or not they have been engaged meaningfully in its design and delivery.
To illustrate the point in a concrete way, we want to share our experience as members of a research team consisting of people who use drugs, legal scholars, physicians, epidemiologists, and others. In May, we were awarded a grant from the Canadian Institutes of Health Research to generate a “scoping review” to synthesize English literature related to safe supply in emergency settings.
Our aim was to identify barriers to, and facilitators of, safe supply, drawing on lessons learned from public health emergencies like SARS or natural disasters such as earthquakes or tsunamis, where extraordinary measures were put in place to improve access to a variety of health care services. With only a month to produce a draft report of our findings, our team got to work, screening thousands of potentially relevant journal articles, including academic literature and grey literature (the latter mainly produced by non-profit organizations). Throughout this work we drew upon the expertise of members of the Canadian Association of People Who Use Drugs (CAPUD) on our research team as well as an expert advisory committee of people who use drugs to ensure that we did not miss any key concepts or search terms critical to assembling a base of relevant materials.
What we found was not that surprising: the published literature has extremely little evidence of how best to provide safe supply in emergency settings. But what we did with that finding underscored the importance of having people who use drugs involved in every aspect of our project.
A standard way of interpreting the lack of evidence would be to simply say “more research is needed.” But the CAPUD members on our team and the advisory committee comprised of people who use drugs pointed out that such a message could easily be misinterpreted to mean that safe supply prescribing should wait until we have more research in hand. Nothing in the literature we analyzed suggested that waiting to act would be beneficial.
The input from people who use drugs highlighted key points that a group of academic scholars could have missed.
Drawing on our collective expertise, and centring the experiences and expertise of the people on the team and committee who use drugs, we instead were clear in concluding that even though more research could help identify and develop strategies to address barriers to safe supply across a range of settings, we do not need any more evidence to know that illicit toxic drugs from unknown sources are unsafe relative to a regulated drug supply.
The input from people who use drugs highlighted key points that a group of academic scholars could have missed. Certified health-care providers have the power to prescribe a safe alternative supply of pharmaceutical drugs and they should do anything in their power to try to save the lives of people who use drugs. Without the guidance of people who use drugs driving our project, that conclusion might have been more muted in our report, such that our findings might have been used for purposes we did not intend and would not support.
Therein lies the power of integrating people who use drugs directly into research as equals and as leaders: they help everyone see the forest for the trees.
There are other ways, too, that the CAPUD members co-leading this project and the advisory group have helped shift the team’s understanding of what purposeful research looks like while ensuring that key evidence and critical considerations for analysis are not missed.
One example relates to the distinction between a “safe” versus “safer” supply of drugs. Many in the field who are otherwise allied with the concerns of people who use drugs point out that “safe” is too strong a word to use because opioids, stimulants, and other substances still carry significant health risks when sourced from a regulated manufacturer. The term “safer supply” is preferred, and we’re beginning to see uptake of this terminology in policy consultations.
That nuance is progress, but for many people who use drugs, including those on our research team, it misses the mark. They argue that conversations about safe supply must expand to take more seriously the prospect of regulating and enabling safe access to all drugs used recreationally. Many prescription drugs are risky to take, but their risks may become better known over time, and alternative treatment options may emerge and be explored in a regulated environment. In contrast, where the only option is an unregulated and often toxic illicit supply, the risk is unquestionable and deadly. This is a point that has fundamentally informed our review and analysis of existing academic and grey literature on safe supply.
In short, meaningful engagement of people who use drugs is necessary to ensure that research intended to address their needs asks the right and sometimes hard questions. For that to happen, people who use drugs must be included and engaged throughout the research process and ultimately the delivery of services such as safe supply.
We have worked to ensure engagement in our project is meaningful, recognizing expertise and contributions to the research by inviting people who use drugs to take on leadership roles in the project, paying the experts an honest wage for their labour, and centring their insights in our analysis and advocacy efforts. We must sustain that approach, and we call upon researchers, service providers, policy-makers, and others who engage with people who use drugs to do the same.
There are resources that can help: for instance, the excellent document Research Manifesto 101, created by community members of Vancouver’s Downtown Eastside. If you are working in the field of drug policy research, or otherwise working to help provide services and/or address the needs of people who use drugs, ask them what their community principles are, who do they need and want representing them, and how they would like to be involved. Securing and sustaining a safe supply for people who use drugs can and should start there.
The CIHR Safe Supply Working Group contributed to this article. It includes Dr. Leah Genge, Dr. Tommy Brothers, Natasha Touesnard, Brianna Cheng, Dr. Ayden Scheim, Dr. Dan Werb, Emilie Comeau, Michael Pugliese and Candis Lepage.
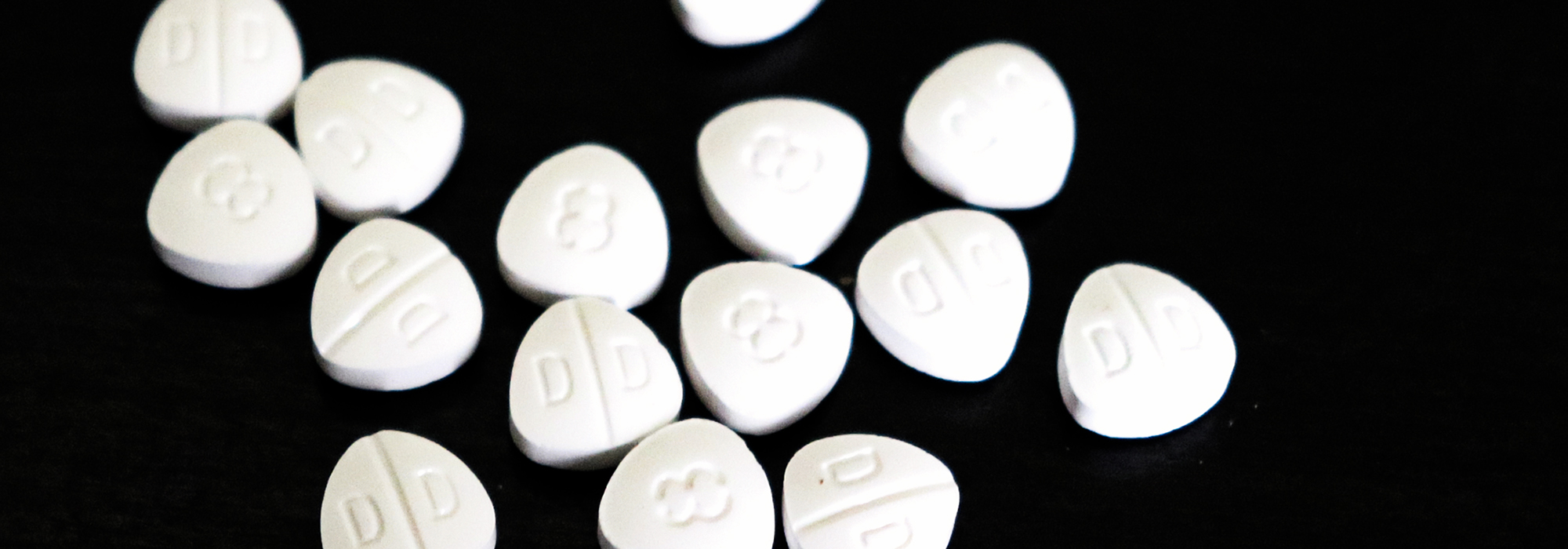
Photo: Dilaudid tablets. Credit: Matthew Bonn.