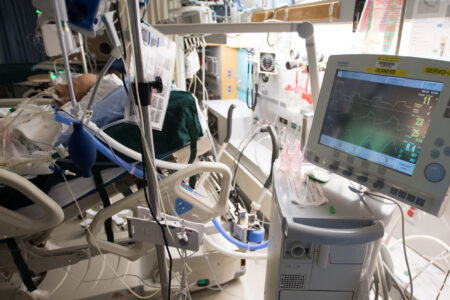
The COVID-19 crisis has brought unique challenges. In times of crises, emergencies, epidemics or wars, an all-of-government approach is vital for effective mobilization of the “whole-of-society.” To be legitimate, credible and effective, policy must be seen to be fair, non-partisan or otherwise skewed. Critical reconsideration of conventional wisdoms to address public health and financial crises is vital as inappropriate policy-making can be costly in many ways.
After the novel coronavirus outbreak in Wuhan, China was first recognized and reported at the end of 2019, the World Health Organization (WHO) designated the outbreak a “public health emergency of international concern” at the end of January, advising all countries to “be ready to contain any introduction of the virus and its spread through active surveillance, early detection, isolation and case management, contact tracing, and prevention.” COVID-19 spread to most developing countries outside Asia in March and April.
However, most governments remained poorly prepared, and only a few, such as relatively poor Vietnam and the state of Kerala in southwest India, adopted sufficient early preventive measures to contain the contagion. Outside of East Asia and Kerala, few insisted on precautionary measures, such as physical distancing and using face masks, early enough to avoid costly lockdowns.
Accustomed to adopting supposed best practices prescribed by rich countries, too many developing country governments have implemented measures without sufficiently taking account of their own circumstances and challenges including resource availability, population distribution and institutional capacities. Some even emulated the initial UK government policy of trying to achieve herd immunity in their populations by allowing contagion to spread.
Lessons from earlier experiences with several major epidemics, such as Severe Acute Respiratory Syndrome (SARS), Middle East Respiratory Syndrome (MERS) and Ebola in recent decades remain uneven, but may be useful to enhance preparedness. However, no standardized set of interventions is likely to be universally valid, let alone applicable, as the pandemic has different ramifications in various circumstances over time.
Unfortunately, health systems in most developing countries can barely cope, even in normal times. Their weak health systems have been further undermined by years of under-investment and selective privatization, often demanded by some donors and international financial institutions. As a result, many fear that the pandemic will have catastrophic consequences.
While an effective vaccine may soon be available, there is no guarantee it will be affordable to most, let alone universally available to all, as with the tuberculosis, polio or smallpox vaccines. Many poor countries cannot afford mass testing, let alone needed personal protective equipment for frontline workers.
As epidemics spread, nationwide lockdowns have typically been imposed indiscriminately, especially hurting poor urban populations with precarious livelihoods, often living in close proximity to one another. In most urban slums, many people live in crammed circumstances, often sharing facilities and much else. This makes physical distancing and other needed measures very difficult.
An economy cannot be locked down for too long because of its devastating implications for livelihoods and incomes. Authorities must choose between the economic disruption of physical distancing and the reckless business-as-usual approach. Much of the population in many developing countries works in the informal sector, often earning variable daily incomes and retaining modest savings.
Viral transmission and infection patterns are shaped by social factors that are both local and intimate, which international and even national public health decision makers are often oblivious to, but which community members may know better. Therefore, joint learning – involving both experts and communities – is vital for designing and improving effective responses.
All too many developing countries believe they do not have enough resources to provide relief for their vulnerable populations, including petty businesses, for extended periods of time. Extending strict lockdown measures is more likely to erode broad public support faster than where adequate social provisioning is assured.
Countries can have less disruptive and costly, yet effective containment strategies, especially if they act early and quickly enough, as timing is critical in the face of the speed and exponential spread of contagion. The ability to trace, test and treat suspected cases, such as those in close recent contact with an infected person, is also crucial.
Effective containment depends heavily on voluntary compliance, community acceptance and trust. This is helped by transparency, health education and shared understanding of what needs to be done. All these require an all-of-government approach, with various components working together and credible, inclusive leadership to mobilize and co–ordinate the whole of society for effective containment. The August resurgence of COVID-19 infections in Kerala and Vietnam underscore the likely need for continued vigilance for a long time to come.
In many situations, public health and police authorities enforce lockdowns with little meaningful consultation with the rest of government, let alone the public. Most ministries and government agencies need to be appropriately engaged to plan, design and implement needed measures.
Success in dealing with this pandemic needs transparent leadership, not only from government, but also from all others involved in whole-of-society mobilization, including community leaders, NGOs and aid agencies, to ensure full public support, cooperation and participation.
Meanwhile, government efficacy depends on credibility which, in turn, requires transparency and demonstrated accountability. Credible explanations of evolving situations and measures undertaken are important for public understanding, cooperation, support and legitimacy.
Flexibility is important, including the willingness and ability to change strategies and policies in response to new developments and knowledge. This is especially true in dealing with rapidly changing situations with so much that is unfamiliar, or worse, misleading.
Singapore’s apparent early success, for example, was not what it seemed as it had overlooked disincentives for infected migrant workers to cooperate with the authorities. Such problems are compounded when sections of a population feel particularly vulnerable to being penalized, especially in dealing with state authorities, e.g., undocumented foreign labour. Credible promises of full amnesties and free medical treatment may help overcome their fears, thus ensuring broader compliance and cooperation.
Diverse, culturally appropriate, enhanced public health and other relevant public communication tools need to be developed and promoted to quickly and effectively mobilise full public engagement. The efficacy of lockdowns and other such measures are often contingent on society’s ability to respond appropriately.
Full social mobilization is undoubtedly needed, but such exceptional emergency or wartime-like measures must not be abused by the temptation to skew implementation for political or financial advantage. Success can be secured by legitimate, credible and inclusive leadership, government and otherwise.
A longer version of this piece can be found in Vulnerable: The Law, Policy and Ethics of COVID-19, edited by Colleen M Flood, Vanessa MacDonnell, Jane Philpott, Sophie Thériault and Sridhar Venkatapuram, out now and available open access from University of Ottawa Press.
This article is part of the Addressing Vulnerabilities for a More Equitable Pandemic Response special feature.