More than 11,000 Canadians have died from COVID-19. As the number of deaths continues to rise, so, too, does the pressure on researchers and biotechnology companies to produce safe and effective vaccines. Fortunately, vaccine research is moving at an unprecedented pace, and it appears that researchers are well on their way to delivering on the promise of a vaccine for COVID-19.
Earlier this month, the Pfizer and BioNTech team, the company Moderna, and the Russian Federation each claimed that their respective vaccines had at least 90 per cent efficacy from interim results of their Phase 3 trials. On Nov. 18, Pfizer and BioNTech announced that they had completed their trial, showing few side effects and 95 per cent efficacy. Pfizer/BioNTech said it would apply to the U.S. Food and Drug Administration (FDA) for emergency approval “within days.”
Notwithstanding this welcome news, the race for safe and effective vaccines continues. Even if all three of these vaccines are approved, production capacity is such that more vaccines are needed to meet the goal of offering vaccination to the nearly eight billion people on the planet. Further, these vaccines are not without problems. For example, Pfizer’s vaccine requires -70C storage, creating significant logistical hurdles.
These limitations explain, in part, the push to accelerate vaccine development using human challenge trials, where healthy volunteers would be deliberately infected with SARS-CoV-2 (the virus that causes COVID-19). This is something that Ontario Liberal MP Marcus Powlowski, and others have championed for months. In late October, Powlowski, a former ER doctor, presented an e-petition to the House of Commons urging the federal government to approve COVID-19 vaccine challenge trials.
While Powlowski and other proponents of challenge trials are well intentioned, their position is misguided. Human challenge trials for the development of a COVID-19 vaccine are unethical and should not proceed in Canada or elsewhere.
With conventional Phase 3 vaccine testing, healthy volunteers receive a candidate vaccine or a salt water injection (placebo). They’re then advised to take precautions to avoid infection as they go about their activities of daily living. The volunteers are followed over time to see who becomes infected and whether there is an appreciable difference between those who received the candidate vaccine and those who received the placebo. The time frame can be shortened if the research participants live in areas with a high rate of infection.
With the proposed Phase 3 vaccine challenge trials, healthy volunteers would receive a candidate vaccine or a placebo, and all would then be deliberately infected with SARS-CoV-2. Following infection, they would be quarantined for a minimum of two weeks to allow researchers to determine whether the vaccine was effective. This approach would considerably shorten the research time frame because there would be no need to wait for chance encounters with the virus.
Recently, the U.K. announced that it expects to proceed with the first steps of a COVID-19 challenge trial in January 2021. Dublin-based clinical-research organizations – Open Orphan and hVIVO – plan to conduct the trial at a high-level isolation unit in north London. The specifics of the trial design have yet to be announced, and approval by an ethical review committee has yet to be obtained.
The first step on the path to a Phase 3 challenge trial involves the production and testing of high-quality GMP-grade coronavirus – virus that is rigorously manufactured according to Good Manufacturing Practice. The next step, which in the U.K. is slated to start in the new year, requires the successful completion of an early-stage dosage-ranging challenge trial. This involves administering very low doses of SARS-CoV-2 to healthy young volunteers, with the dose slowly increased until the researchers have determined the dose that reliably infects persons. Then comes the Phase 3 challenge trial where the volunteers get a candidate vaccine or placebo before being intentionally infected with the virus.
One of the many concerns with Phase 3 COVID-19 vaccine challenge trials is the absence of rescue treatments in the event that a research participant becomes seriously ill. While vaccine challenge trials for other infectious diseases, including malaria, influenza, and cholera, have been implemented to great benefit, these diseases have reliable treatments. This is not yet the case for COVID-19.
Another concern is the problem of extrapolation. The proposed target population for COVID-19 vaccine challenge trials is youth between the ages of 18 to 30 as they are believed to be among those least likely to experience the more serious harmful effects of infection. But a vaccine that works well in a lower-risk group – healthy young adults – may not work the same way in other groups. In Canada, for example, a majority of the health problems are experienced by older adults and the majority of deaths are among those in long-term care facilities. These are very different populations from those that would be included in a challenge trial. With conventional vaccine trials, research is conducted in a more diverse age group, including high-risk populations.
Additionally, there are concerns about the twin risks of exploitation and coercion. It has been suggested that healthy volunteers in the U.K. would be paid around £4,000 (C$7,000) for their time. For some volunteers, money is an important benefit of research participation, but how does this weigh against the risk of death or possibly chronic, catastrophic illness? Is $7,000 too little or too much money? Further, might this sum be more enticing for the target population, who may be more in need of funds due to pandemic-related rising unemployment? At the very least there is the risk of undue inducement.
Added to these issues is the fact that the background conditions have changed dramatically since COVID-19 vaccine challenge trials were first proposed. There are now 57 candidate vaccines in clinical trials. Twelve of these are currently in large-scale conventional Phase 3 trials. The company behind one of these 12 is on the cusp of seeking regulatory approval from the FDA, and two others have posted promising results.
The perceived need to speed up COVID-19 vaccine development using challenge trials is no longer pressing. If there ever was a sound reason to proceed with such trials, that time has surely passed.
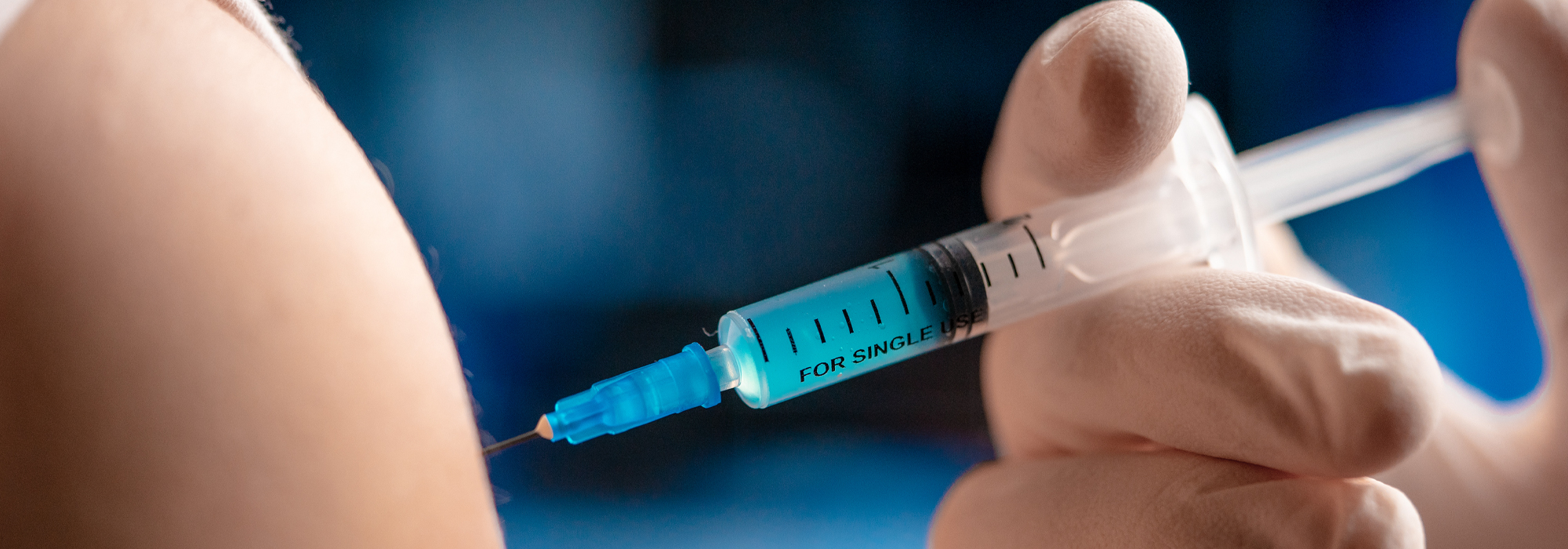
Photo: Shutterstock/By Akaberka